The biggest reason custom EHR projects fail is not bad engineering. It’s a correct architecture built for the wrong problem.
Most teams spend the first three months designing a clinical documentation experience that physicians will love. Clean note templates, intuitive scheduling, a patient timeline that actually makes sense.
They get that part right. Then they hit the HIPAA audit logging requirement, the HL7 v2 lab interface, and the ONC certification testing cycle and discover that the work they thought was 70% complete was actually 30% complete.
The hard parts of custom EHR software development are invisible during planning. They don’t show up in wireframes. They don’t appear on a feature list. And most software development vendors either don’t know to price them in or choose not to, because the project wouldn’t close if they did.
EngineerBabu, a CMMI Level 5 product engineering firm, has built financial infrastructure for EarlySalary (now processing ₹10,000 crore in disbursements), AI-powered field intelligence for Simba Beer, and the full lending stack for LoanOS across 7 modules.
Healthcare products present a different class of constraint regulatory, clinical, and interoperability requirements that compound on each other. This guide is what I wish I could hand every CTO or founder before they write their first line of architecture for an EHR.
What Is Custom EHR Software Development?
Custom EHR software development is the process of designing, building, and deploying an Electronic Health Record system from the ground up or extending an existing platform to fit specific clinical workflows, patient data models, specialty requirements, and integration landscapes, rather than purchasing an off-the-shelf system like Epic, Cerner, or athenahealth.
A custom EHR typically includes a patient chart management system, clinical documentation tools, appointment scheduling, prescription management (e-prescribing), lab and imaging order management, and a provider portal. More sophisticated builds add billing and revenue cycle management, telehealth modules, population health analytics, patient engagement portals, and payer integrations.
The decision to build custom versus license an off-the-shelf solution is not a technology decision. It’s a business model decision.
The Problem Most CTOs Underestimate by 3 to 4 Times
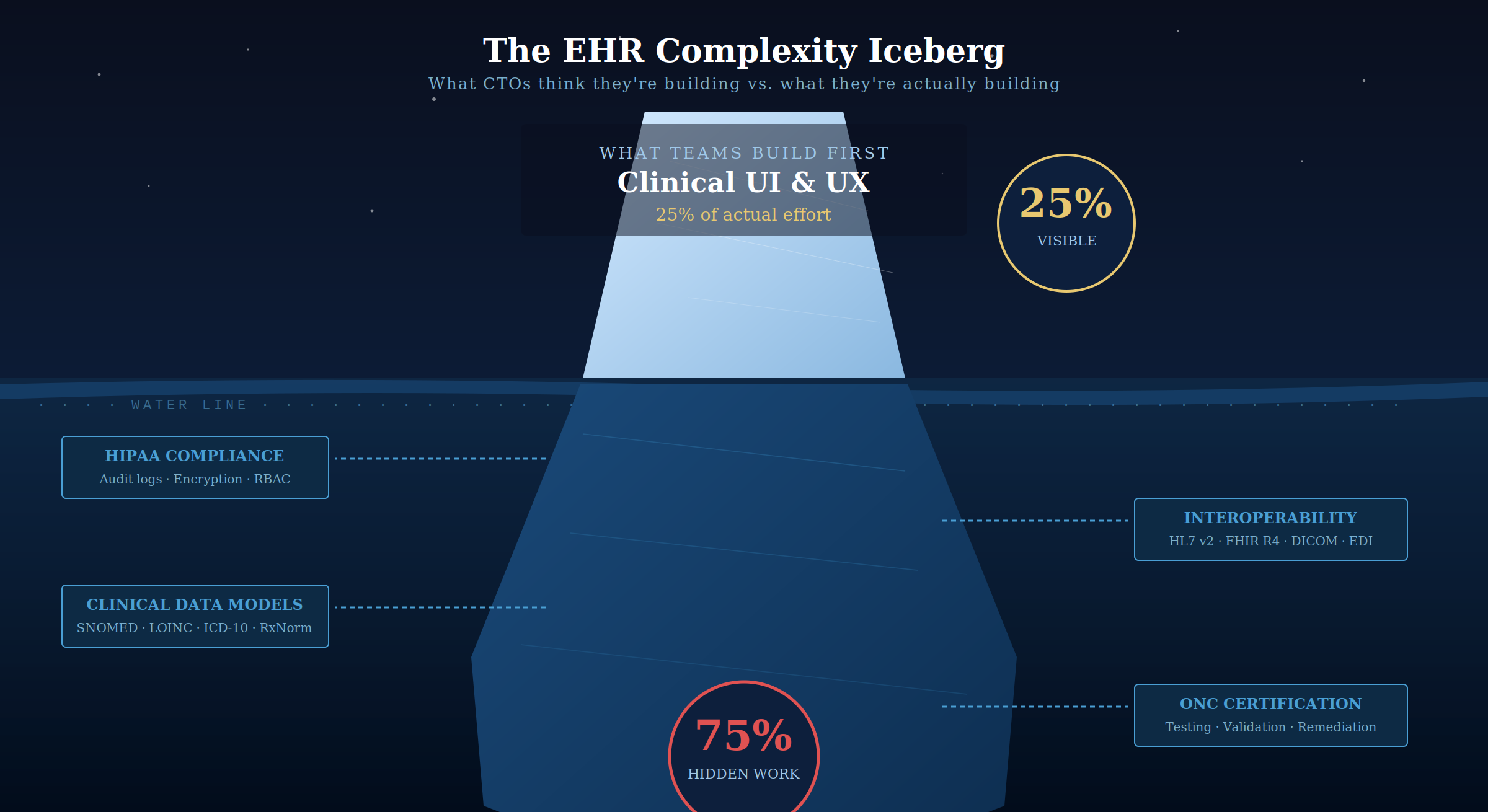
Every CTO who comes to me with an EHR development brief has already solved the wrong problem. They’ve thought carefully about the frontend, the clinical documentation experience, the appointment calendar, the patient timeline view. That work matters. But it’s typically 25% of the actual development effort.
The other 75% lives in four areas that rarely appear on a pre-sales scope document:
- HIPAA compliance architecture: Role-based access control, PHI encryption at rest and in transit, audit logs for every data access event, automatic session timeout, breach notification workflows. This is not a feature. It’s a foundational architectural decision that costs 2 to 3 times more to retrofit than to build in from day one.
- Interoperability: HL7 v2, HL7 FHIR R4, CDA documents, IHE profiles. Every lab network, pharmacy chain, imaging center, and payer your system needs to talk to has its own integration quirks. I’ve seen a single PACS system integration add 6 weeks to a timeline because of a non-standard DICOM implementation.
- Clinical data models: SNOMED CT, LOINC codes, ICD-10, CPT codes, RxNorm. Your database schema is not just columns and rows — it’s a terminological system that has to interoperate with every external system in the ecosystem.
- ONC certification testing: If your clients will bill Medicare or Medicaid, you almost certainly need ONC 2015 Edition Cures Act certification. Testing involves external certification bodies, test data sets, and multiple validation rounds. Most development vendors don’t price this in.
According to HIMSS 2025 data, EHR integration and interoperability failures account for 34% of healthcare IT project overruns. In my experience reviewing these projects, that number is low, it doesn’t capture the indirect delays from interoperability gaps that appear post-launch.
Custom EHR Architecture: The Stack Decisions That Actually Matter
I’ve reviewed EHR codebases built on ten different stacks. Some of the worst clinical software I’ve seen was built on technically excellent infrastructure. The stack is not the differentiator. The architecture decisions within the stack are.
-
Backend: Microservices vs. Modular Monolith
The microservices-versus-monolith debate in EHR development is usually decided by the wrong factor: what’s trendy. Here’s the honest answer. If you’re building a single-specialty EHR for under 50 providers, a well-structured modular monolith (Node.js or Python FastAPI) will serve you better than microservices for the first 3 to 4 years.
The operational overhead of orchestrating 12 microservices — service mesh, distributed tracing, API gateway, inter-service authentication — is substantial, and for a 10-developer team it’s often counterproductive.
If you’re building a multi-tenant, multi-specialty platform that needs to independently scale the clinical documentation module from the billing module, microservices earn their complexity. The rule of thumb I use: microservices are justified when different modules have meaningfully different scaling profiles and genuinely different deployment cadences.
-
Database: PostgreSQL for Clinical Data
PostgreSQL is the right choice for core clinical data. Full stop. FHIR resources map cleanly to relational schemas with JSONB columns for flexible resource extensions. The ACID compliance matters enormously when you have concurrent writes from nurses, physicians, and care coordinators on the same patient chart. MongoDB is fast for document reads but the flexibility of a schema-less design is a liability when your data model has to conform to SNOMED CT and LOINC standards.
Elasticsearch or OpenSearch as a secondary index for clinical search is a strong addition. Real-time typeahead search across medication names, diagnosis codes, and patient records on top of PostgreSQL full-text search is not fast enough at scale.
-
FHIR Server: Build or Buy
Do not build your own FHIR server. This is one of the clearest build-versus-buy decisions in EHR development. HAPI FHIR (open source, Java), Azure Health Data Services, Google Cloud Healthcare API, and AWS HealthLake are all production-grade options. Each has tradeoffs in cost, control, and vendor lock-in. The 3 to 6 months you’d spend building a custom FHIR R4 server is better spent on clinical workflow differentiation.
-
Authentication and PHI Access Control
OAuth 2.0 with SMART on FHIR is the standard for clinical application authorization. If you’re building a patient-facing portal, SMART on FHIR handles the scoped access model (a patient app that can read but not write, or a provider app with write access to specific resource types). Every PHI access event needs to write to an immutable audit log. Every row. Every request. This is not optional under HIPAA’s Technical Safeguards rule.
Architecture Stack Reference Table:
| Architecture Layer | Recommended Choice | Alternative | Why It Matters for EHR |
| Core API | Node.js (Fastify) or Python FastAPI | Java Spring Boot | FHIR API performance at scale |
| Clinical Database | PostgreSQL 16+ | MySQL | JSONB for FHIR resources, ACID compliance |
| FHIR Server | HAPI FHIR / Azure Health Data Services | Custom build | ONC certification, interoperability |
| Search | Elasticsearch / OpenSearch | Postgres full-text | Clinical typeahead, medication search |
| Auth | OAuth 2.0 + SMART on FHIR | Custom JWT | HIPAA access control, patient consent |
| Messaging/Events | RabbitMQ or AWS SQS | Kafka (overkill at MVP) | Lab results, HL7 ADT events, alerts |
| Infra | AWS (HIPAA eligible) or Azure | GCP Healthcare API | BAA availability, HIPAA eligible services |
| Frontend | React + TypeScript | Next.js for SEO-heavy portals | Complex clinical UI state management |
HIPAA Compliance in Custom EHR Development: It’s an Architecture Decision, Not a Checklist
I’ve had clients come to me with EHR builds that were six months in and suddenly needed to “add HIPAA compliance.” The conversation never goes well. HIPAA compliance is not a layer you add on top of a working system. It’s a constraint that shapes every layer of your stack from the first sprint.
The HIPAA Security Rule has three categories of safeguards: Administrative, Physical, and Technical. Software development addresses the Technical Safeguards. Here’s what those actually translate to in a custom EHR build:
- Access controls: Unique user identification, emergency access procedures, automatic logoff after inactivity (typically 15 to 30 minutes), encryption and decryption of ePHI.
- Audit controls: Hardware, software, and procedural mechanisms to record and examine activity in systems that contain PHI. In practice: immutable audit logs for every read, write, update, or delete operation on any PHI-bearing record.
- Integrity controls: Mechanisms to authenticate ePHI to ensure it has not been altered or destroyed in an unauthorized manner. Cryptographic checksums, database transaction logs.
- Transmission security: TLS 1.3 for all data in transit, AES-256 encryption at rest. Every API endpoint. Every file storage bucket. No exceptions.
- Business Associate Agreements (BAA): You need a BAA with every infrastructure vendor that touches PHI. AWS, Azure, Google Cloud, Twilio (if you send SMS), SendGrid (if you send email with PHI). Every one. Document each BAA in your compliance records.
HL7, FHIR R4, and the Interoperability Reality Nobody Talks About
The 21st Century Cures Act mandated information blocking prohibitions and FHIR R4 API requirements for certified EHR technology. In practice, this means your custom EHR must expose a FHIR R4 API that allows patients and authorized third-party applications to access their health data. This is not optional for ONC-certified systems.
What nobody tells you in the early planning conversations is that interoperability has three separate complexity layers, each one more expensive than founders estimate:
- External system integration: Lab networks (Quest Diagnostics, LabCorp, local reference labs) typically speak HL7 v2.x over MLLP. That means maintaining a legacy HL7 listener alongside your modern FHIR API. Pharmacy networks use NCPDP SCRIPT. Imaging systems speak DICOM. Payer systems use X12 EDI 837 for claims. None of these are FHIR. Budget 4 to 8 weeks per major external integration.
- Patient data sharing: USCDI (United States Core Data for Interoperability) defines the minimum dataset that must be available via FHIR API. Your FHIR API must support at minimum the USCDI v3 data classes as of 2024 requirements. This drives your clinical data model design.
- Care coordination: Referral management, care transitions, and direct messaging (Direct Protocol) for provider-to-provider communication. Often overlooked at MVP stage, always required by the time you’re in production with multi-provider clients.
The practical implication: your development team needs at minimum one engineer with dedicated healthcare interoperability experience. This is a rare skill set. A general full-stack developer who is excellent at building APIs will underestimate this work significantly — not from incompetence, but from not knowing what they don’t know.
Build vs. Buy vs. Extend: The Decision Framework I Use With Every Healthcare Client
The build-versus-buy decision in EHR is more nuanced than most content on this topic acknowledges. There are three real options: build from scratch, license and white-label an existing platform, or extend an open-source EHR like OpenMRS or OpenEMR. Here’s how I think through each scenario.
| Scenario | Best Path | Time to Market | Typical Cost Range | Control Level |
| Single specialty clinic going digital | Off-the-shelf (Kareo, DrChrono) | 2 to 6 weeks | $200 to $800/month | Low |
| Digital health startup with niche clinical workflow | Custom development (MVP) | 8 to 12 months | $120K to $200K | Full |
| Health system needing integrations only | Extend existing EHR via FHIR API | 3 to 6 months | $40K to $90K | Medium |
| White-label telehealth with EHR | White-label platform + custom skin | 2 to 4 months | $25K to $70K | Medium |
| Platform business (EHR-as-product) | Custom from scratch | 14 to 24 months | $300K to $600K+ | Full |
| LMIC market or underserved setting | Extend OpenMRS or OpenEMR | 4 to 8 months | $60K to $140K | High |
The signal I look for: if the EHR is your core product and your clinical workflow is genuinely differentiated, build custom. If the EHR is infrastructure that enables your real value proposition (e.g., a population health analytics layer on top of clinical data), there’s a strong argument for starting with an open-source foundation or a FHIR-enabled platform.

Custom EHR Development Cost and Timeline: Real Numbers, Not Ranges
Every article on this topic gives you the same useless range: “$10,000 to $500,000.” That’s not a cost estimate. That’s a way of saying “I don’t know.” Here’s how I actually think about EHR development cost.
Cost Drivers, Ranked by Impact
- Number and complexity of external integrations — Each lab network, pharmacy system, imaging center, or payer integration adds $15,000 to $35,000 in development cost and 4 to 8 weeks to timeline.
- HIPAA compliance scope — A properly architected HIPAA compliance layer (audit logging infrastructure, encryption key management, BAA administration, penetration testing) costs $20,000 to $40,000 across a full EHR project.
- ONC certification — If required, add $40,000 to $80,000 and 3 to 6 months for certification testing, remediation, and documentation.
- Clinical data model complexity — Building for a single specialty with a defined data model is 40% cheaper than building a multi-specialty platform with extensible clinical data models.
- Team composition — US-based development teams: $180 to $300/hour blended. India-based CMMI Level 5 teams with healthcare domain experience: $45 to $80/hour blended. The cost differential over an 18-month project is material.
Module-by-Module Timeline
- Discovery and Architecture (6 to 8 weeks): Clinical workflow analysis, data model design, integration mapping, HIPAA compliance architecture, technology stack finalization. Do not skip or compress this phase. It determines 80% of downstream costs.
- Core Clinical Infrastructure (10 to 14 weeks): Patient demographics, clinical note framework, FHIR R4 server setup, authentication and RBAC, PHI encryption and audit logging. This is the foundation everything else sits on.
- Clinical Modules (12 to 18 weeks): Appointment scheduling, clinical documentation, medication management (e-prescribing), lab/imaging orders, problem list, vital signs, care plan. Each module is 3 to 6 weeks.
- External Integrations (8 to 20 weeks, depends on scope): Lab network HL7 v2 integration, e-prescribing (Surescripts or DrFirst), patient portal, payer connectivity. Each integration has its own testing requirements.
- Revenue Cycle and Billing (8 to 12 weeks, if in scope): ICD-10/CPT coding, claim generation (X12 837), ERA/EOB processing (X12 835), patient statement management. This module alone accounts for 20 to 25% of total project cost when included.
- ONC Certification Testing (12 to 24 weeks, if required): Automated measure testing, clinical quality measure validation, accessibility testing (Section 508), external certification body review. Run this in parallel with other development if possible.
What Most EHR Development Articles Get Wrong
I’ve read enough content on this topic to recognize the patterns. Here are the things that are either underweighted or flatly wrong in most of what you’ll find:
Wrong: HIPAA compliance is a security layer you add before launch.
HIPAA compliance is an architectural foundation. The audit logging alone — capturing every PHI access event, storing it immutably for 6 years under HIPAA’s retention requirements — affects database schema design, API middleware architecture, and storage cost modeling from the first sprint.
Wrong: You need a microservices architecture to build a scalable EHR.
The most clinically impactful EHRs I’ve seen, serving tens of thousands of patients, run on well-structured modular monoliths. The complexity cost of microservices does not pay for itself until you have a team of 15 to 20 engineers and genuinely different scaling profiles per service.
Wrong: Off-the-shelf integration with existing EHRs is straightforward.
Every health system has a version of Epic or Cerner that has been customized for 15 years. Their FHIR R4 APIs are certified, but the data quality in those systems is not. Duplicate patients, legacy codes, missing demographics — plan for a data quality layer in any integration project.
Underweighted: Clinical adoption is a UX problem, not an engineering problem.
The most technically sound EHR will fail if physicians find it adds 20 minutes to their daily documentation burden. The build process should include clinical workflow observation (shadowing providers), UX prototype testing with actual clinicians, and a clinical advisory board that reviews UI decisions before development.
“I’ve watched technically excellent EHR builds fail in production because the team optimized for FHIR conformance and forgot to optimize for the physician who has 15 patients to see before noon.”
Underweighted: Post-launch regulatory maintenance.
The ONC updates certification requirements. HIPAA enforcement interpretations evolve. ICD-10 codes are updated annually. A custom EHR is not a build-it-and-leave-it product. Budget 15 to 20% of initial development cost annually for maintenance, updates, and regulatory compliance work.
If You’re Evaluating a Custom EHR Build
If you’re in the architecture evaluation phase weighing custom build against white-label, trying to scope HIPAA and ONC requirements, or figuring out whether your existing development partner has genuine healthcare interoperability experience.
I’m usually the one on those calls at EngineerBabu.
I don’t have a sales team. I do 20 projects a year and every one starts with a direct technical conversation. If you want to talk through the architecture decisions before you commit to a vendor, reach out.
Mayank Pratap Co-founder of EngineerBabu. 14 years building technology products. Led product architecture on 500+ projects across 20+ countries, including 75 YC-selected builds and 4 unicorn client products. Google AI Accelerator Top 20 (2024). Backed by Vijay Shekhar Sharma (Paytm founder). NASSCOM member. Harvard Innovation Labs participant.
CMMI Level 5 | Google AI Accelerator Top 20 | LinkedIn Top 20 Startups India | NASSCOM Member | 500+ Projects Delivered | Harvard Innovation Labs
Frequently Asked Questions
-
How much does custom EHR software development cost?
Custom EHR development typically costs between $80,000 and $500,000+ depending on scope. A 4-module MVP development with HIPAA compliance, HL7/FHIR integration, and a clinical portal runs $120,000 to $180,000 over 8 to 12 months.
Full-scale enterprise EHR with billing, telehealth, and advanced analytics runs $350,000 to $600,000+. The biggest cost variable is the number of external integrations and whether ONC certification is required.
-
How long does it take to build a custom EHR system?
An MVP EHR takes 6 to 10 months. A production-grade, multi-specialty EHR with HIPAA audit trails, interoperability, and billing integration takes 14 to 24 months.
The variance usually comes from underestimating third-party integrations labs, PACS, pharmacy, and payer systems each add 4 to 8 weeks. ONC certification testing adds another 3 to 6 months if required.
-
What does HIPAA compliance require in EHR development?
HIPAA compliance in EHR development requires PHI encryption at rest and in transit (AES-256, TLS 1.3), role-based access control, audit logging for every PHI access event, automated session timeouts, and a Business Associate Agreement with all infrastructure vendors.
It’s an architecture decision made on day one, not a feature added before launch. Retrofitting costs 2 to 3 times more than building it in from the start.
-
What technology stack is best for custom EHR development?
For most EHR builds: Node.js or Python FastAPI on the backend, PostgreSQL for clinical data, Redis for caching, HAPI FHIR or Azure Health Data Services as the FHIR server, React with TypeScript on the frontend, deployed on AWS or Azure with HIPAA-eligible services.
FHIR R4 is the interoperability standard. Do not build your own FHIR server — use an existing implementation.