I recently sat across from a hospital CTO who had spent 18 months and $180,000 building an EMR system in-house. It wasn’t live yet. Not a single doctor had used it.
His engineering team had rewritten the patient record module three times because nobody told them upfront that HL7 FHIR R4 compliance isn’t optional if you want to connect with insurance systems. The fourth rewrite was happening when we spoke.
That’s not a horror story. That’s Tuesday in healthcare software.
The difference between a functional EMR and an expensive shelf item usually comes down to one decision made at the start: who you’re building with, and whether they’ve shipped healthcare software before or just claim they have.
I’m Mayank Pratap, co-founder of EngineerBabu.
We’re a CMMI Level 5 product engineering company, recognized by Google AI Accelerator (Top 20 globally, 2024), NASSCOM, and LinkedIn Top 20 Startups India.
We’ve shipped 500+ products across 20+ countries, including fintech platforms now processing thousands of crores in transactions. Healthcare is one of the verticals where we go deep, not wide.
This is my honest breakdown of what EMR software development actually costs, how long it actually takes, what the architecture decisions actually look like, and how to pick a company in India that won’t waste your money.
What Is EMR Software Development and Why India Makes Sense for It
EMR software development is the process of designing, building, and deploying Electronic Medical Records systems that allow healthcare providers to create, store, manage, and share patient health data digitally.
A modern EMR system includes clinical documentation, patient scheduling, prescription management, lab order workflows, billing integration, interoperability via HL7/FHIR standards, and increasingly AI-assisted clinical decision support.
Why India specifically? Not because it’s cheap. Because the talent density for healthcare-adjacent software has grown sharply in the last 5 years.
India’s IT services sector crossed $254 billion in revenue in FY2024 (NASSCOM), and a significant portion of that growth is in regulated industry software, including healthcare, fintech, and insurtech.
The engineers who built banking-grade compliance systems for fintech companies are the same ones who understand audit trails, data integrity, and regulatory architecture in EMR systems.
Cost is a factor, but it’s the secondary factor. The primary factor is finding a team that’s actually done this before.
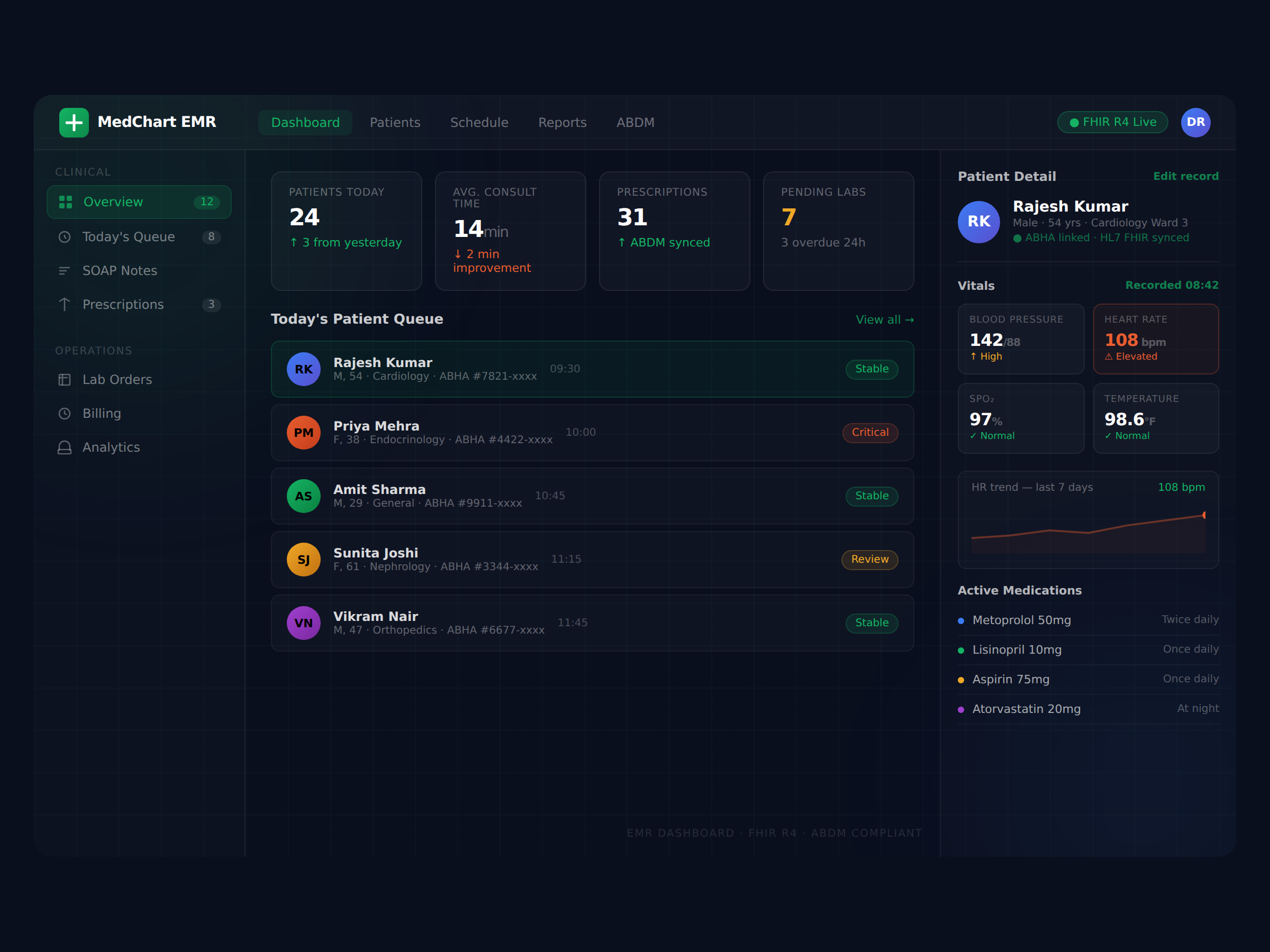
The Real Cost of Building EMR Software in India
Most CTOs I talk to underestimate the budget by 3-4x. They come in expecting ₹20-30 lakhs for an MVP development and leave the conversation understanding why a production-ready EMR starts at ₹60-120 lakhs for a focused build.
Here’s why:
-
Compliance is not an afterthought
HIPAA (if you’re building for US clients), ABDM compliance (for India’s Ayushman Bharat Digital Mission), HL7 FHIR R4, and SNOMED-CT/ICD-10 coding aren’t features you sprinkle on top.
They shape your entire data architecture. If your vendor quotes without asking about compliance requirements in the first call, that’s your signal to walk.
-
Integration complexity compounds
A typical mid-size hospital EMR connects to: a PACS/RIS system for radiology, a LIS for pathology, a pharmacy management system, an insurance/TPA portal, a government health registry, and billing software.
Each of these integrations is 3-6 weeks of work at a minimum. A vendor who quotes without scoping integrations is quoting for a system that won’t function in the real world.
Here’s a realistic budget framework by scope:
| EMR Build Type | Scope | Estimated Cost (INR) | Timeline |
| Department-level MVP | Single specialty, basic records + scheduling | ₹40-70 lakhs | 5-7 months |
| Mid-size hospital EMR | Multi-department, ABDM-compliant, basic integrations | ₹90-160 lakhs | 9-14 months |
| Enterprise EMR Platform | Multi-facility, full interoperability, and AI features | ₹2-5 crores | 18-30 months |
| White-label EMR SaaS | Multi-tenant, configurable per hospital | ₹1.5-4 crores | 14-24 months |
These aren’t padded estimates. They’re what it takes to build something a doctor will trust with patient data.
Core Modules That Determine Whether Your EMR Gets Used or Abandoned
I’ve seen technically sound EMR systems that doctors refused to use after go-live. Not because they were buggy.
Because the clinical workflow design was built by engineers who had never watched a doctor work.
The modules that determine adoption:
-
Patient Registration and Demographics
This is the front door. If registration takes more than 90 seconds, front desk staff find workarounds. The UX here needs to be built with actual registration clerks in the room, not from a requirements document.
-
Clinical Documentation and SOAP Notes
Free-text entry with structured templates. Voice-to-text integration is no longer a nice-to-have.
According to a 2025 survey by KLAS Research, 67% of physicians cite documentation time as their primary driver of burnout. An EMR that adds to documentation time will get rejected inside 6 months.
-
Prescription Management and Drug Interaction Checks
This needs real-time drug interaction databases (Multum, First Databank, or equivalent). Skipping this is a patient safety issue, not just a feature gap.
-
Lab Order Management and Results Viewing
Bidirectional LIS integration. Orders go out, results come back, and abnormal flags surface automatically. Anything less than this creates manual reconciliation work that eats a lab technician’s entire morning.
-
Appointment Scheduling and Patient Portal
In 2025, patients expect self-scheduling, digital intake forms, and appointment reminders via WhatsApp or SMS.
A 2025 report by Deloitte Healthcare found that hospitals with patient self-service portals saw 23% reduction in no-show rates.
-
Billing and Insurance Claims
ICD-10 coding, claim scrubbing, rejection management. The billing module is where EMR projects die in India. Most developers underestimate how hospital billing workflows vary by facility type, specialty, and state.
The Architecture Decisions That Separate Good EMR Vendors from Expensive Mistakes
This is the section that competitors won’t write because they haven’t made these calls in production.
-
Monolith vs. Microservices
For a single-hospital deployment under 200 concurrent users, a well-structured monolith with modular internal architecture is faster to build, easier to maintain, and cheaper to host.
I push back on teams that want microservices for an EMR MVP. The operational overhead is not worth it at that scale.
Microservices make sense when you’re building a multi-tenant SaaS EMR platform serving 50+ hospitals. Know the difference before the architecture review.
-
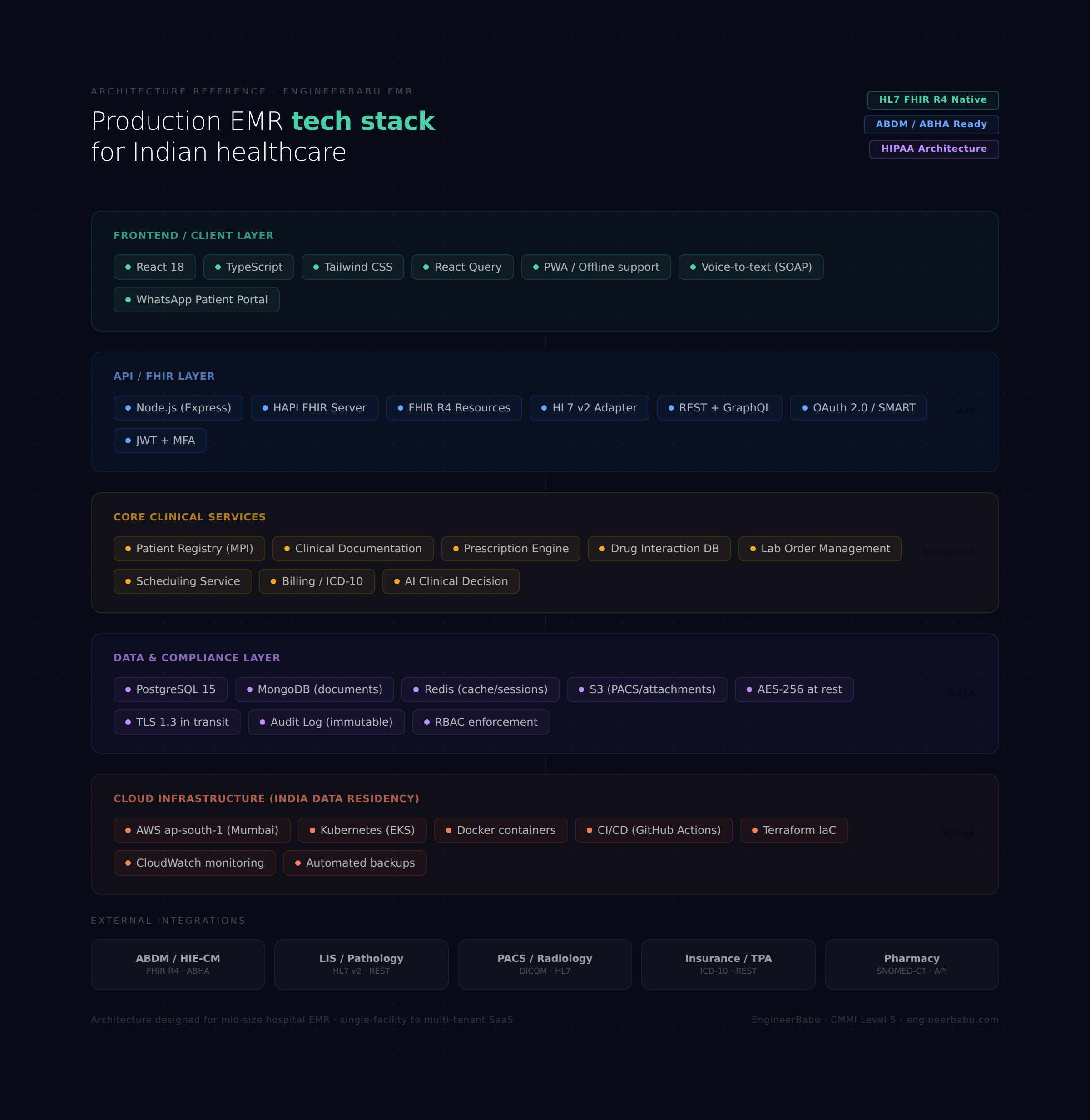
Database Architecture
PostgreSQL as the primary data store for structured clinical data, with document storage (MongoDB or S3-backed blob storage) for unstructured attachments like scan images, discharge summaries, and uploaded PDFs.
Mixing these appropriately is a judgment call. Teams that use a single NoSQL database for everything haven’t dealt with audit trail requirements in a regulated environment.
-
FHIR API Layer
If you’re building for interoperability (and you should be), your FHIR R4 server needs to expose resources including Patient, Encounter, Observation, MedicationRequest, DiagnosticReport, and Appointment.
This layer is not just for government compliance. It’s what lets you connect to insurance portals, referral networks, and national health exchanges without custom point-to-point integrations for every connection.
-
Cloud Hosting and Data Residency
For ABDM compliance in India, patient data must remain within Indian territory. AWS Mumbai (ap-south-1) or Azure India Central are the standard choices.
Government health projects sometimes require NIC Cloud or private cloud deployment. Confirm data residency requirements before you sign anything with a hosting provider.
-
Role-Based Access Control and Audit Logging
Every record access, every modification, every data export needs to be logged with timestamp, user identity, and action type.
This isn’t a feature for large hospitals only. A 3-doctor clinic with one EMR incident where patient data was accessed without authorization faces the same regulatory exposure. Build RBAC and audit logging from day one, not as a retrofit.
-
Encryption Strategy
AES-256 at rest, TLS 1.3 in transit, field-level encryption for sensitive identifiers like Aadhaar numbers. If a vendor doesn’t bring up encryption specifics in a technical discussion, that’s a red flag.
What the EngineerBabu Team Learned Building Healthcare and Fintech Systems
When the EngineerBabu team built EarlySalary’s lending platform, now processing ₹10,000 crore in disbursements, the core lesson was: compliance infrastructure and core product architecture are the same decision.
You can’t separate them. The same principle applies harder in healthcare, where the stakes aren’t just financial penalties but patient safety.
In one healthcare engagement we took on, a mid-size diagnostic chain needed to replace a legacy on-premise EMR with a cloud-native system across 12 centers. The previous vendor had delivered a system that worked in isolation at one center.
The moment they tried to centralize patient records across locations, the data model broke down. There was no unified patient ID strategy, no master patient index, and no deduplication logic.
We spent 6 weeks in data archaeology before writing a line of new code.
The lesson:
Ask any EMR vendor how they handle patient identity management across multiple facilities. If they haven’t built multi-facility systems before, their single-facility system will create migration debt the moment you grow.
Another pattern I see repeatedly: teams that underestimate the effort of clinical change management. You can build a technically perfect EMR and still fail implementation. Doctors have workflow muscle memory built over the years.
The go-live strategy, training design, and 30-day hypercare support period are as important as the software itself.
How to Evaluate an EMR Software Development Company in India
Before you sign a contract or pay a rupee, run this evaluation:
1. Technical Depth Questions (ask these in the first call):
- What FHIR version do you build against, and which resources have you implemented in production?
- How do you handle duplicate patient records in a multi-facility deployment?
- What’s your approach to database schema versioning and zero-downtime migrations?
- Have you integrated with ABDM Health Records (HIE-CM) before?
If the answers are vague, move on.
2. Process and Accountability Questions:
- Who will be on the architecture review call? (If no senior engineer is on the first call, that’s what you’re getting throughout the project.)
- What’s your process when a compliance requirement surfaces mid-build that wasn’t in the original scope?
- Can I talk to a reference client who has taken their EMR to full production, not just UAT?
3. Red Flags to Watch:
- Fixed-price quotes delivered within 24 hours without a discovery session
- “We’ll handle HIPAA/ABDM compliance” without specifics on how
- Portfolio that shows UI mockups but no production metrics
- No one on the team with healthcare industry domain experience
- Offshore teams where the person you talk to pre-sale isn’t the person building your product
4. What a Good Engagement Looks Like:
- 2-4 week paid discovery phase before the build quote
- Architecture decision document delivered before development starts
- Bi-weekly demo cycles, not quarterly milestone reviews
- Compliance requirements documented as acceptance criteria, not footnotes
- Clear handoff documentation for your internal team post-launch
Build vs. Buy vs. Customize: The Decision Framework
This question comes up in every healthcare tech conversation I have. Here’s how I think about it:
1. Buy an off-the-shelf EMR when:
- You’re a small clinic (under 10 providers) with standard workflows
- You don’t need custom integrations or white-labeling
- Speed to implementation matters more than differentiation
- Budget is under ₹10 lakhs per year
Options in India: Practo, Lybrate for Business, DocPulse, eVitalRx for pharmacy.
2. Build custom when:
- You’re building a product to sell to hospitals (SaaS development/platform play)
- Your clinical workflows have genuine differentiators
- You need deep integration with proprietary systems
- You’re a hospital group with 5+ facilities needing centralized data
3. Customize an open-source base when:
- You want FHIR-native infrastructure without building from scratch
- Timeline is under 12 months but scope is mid-size
- Your team has in-house developers who can maintain it
OpenMRS and GNU Health are the two most credible open-source EMR bases for Indian deployments.
Be realistic about customization costs: significant customization of OpenMRS often costs 60-80% of what a clean custom build would cost, but you start with battle-tested clinical data models.

What Most People Get Wrong About EMR Development in India
The biggest mistake isn’t picking the wrong vendor. It’s skipping the requirements phase to save money.
I’ve watched companies spend ₹8-12 lakhs on a “requirements document” with a consultancy and then argue it was wasted money. That document is what keeps a ₹1.5 crore build from becoming a ₹3 crore rebuild.
The second mistake: assuming your IT team can manage an EMR implementation as a side project. EMR go-lives need a dedicated internal project owner with clinical credibility, someone doctors will listen to when there’s resistance.
This is not an IT project. It’s a clinical operations project that IT enables.
Third: underestimating data migration. If you’re replacing a legacy system, the cost and time of migrating legacy patient records into a FHIR-compliant data model is often 20-30% of the total project budget.
It needs its own workstream, its own timeline, and its own QA protocol. Vendors who bundle it into “implementation” without a separate breakdown haven’t done it before.
Fourth: skipping pilot deployment. Every EMR I’ve seen go live successfully went through a 4-6 week pilot at one ward, one department, or one facility before full rollout.
Every one that went straight to full rollout had a painful first 60 days.
Before You Pick a Vendor, Let’s Talk Architecture
If you’re evaluating EMR software development and want to work through the architecture decisions, compliance scope, and build-vs-buy calculus before you commit to anything, I’m usually the one on those calls at EngineerBabu.
We take 20 projects a year. No sales team. No account managers. If I think your project is better served by an off-the-shelf solution or an open-source base, I’ll tell you that in the first conversation.
If it’s the kind of build we can genuinely help with, we’ll show you exactly how we’d approach it.
No pitch deck. No follow-up email sequence. Just a direct conversation.
————————————————————————————————————————–
Mayank Pratap is the co-founder of EngineerBabu, a CMMI Level 5 product engineering company recognized by Google AI Accelerator (Top 20 globally, 2024) and LinkedIn Top 20 Startups India.
He has 14 years of experience building technology products across fintech, healthtech, and enterprise SaaS, with 500+ projects delivered across 20+ countries.
Frequently Asked Questions
-
How long does it take to build an EMR from scratch in India?
A focused department-level EMR MVP takes 5-7 months from requirements sign-off to go-live. A full hospital EMR with multi-department workflows, ABDM compliance, and core integrations takes 9-14 months.
Enterprise multi-facility platforms should budget 18-30 months. These timelines assume a discovery phase is completed before development starts.
-
What is ABDM compliance and does my EMR need it?
ABDM stands for Ayushman Bharat Digital Mission, India’s national digital health infrastructure.
ABDM compliance means your EMR can generate and link ABHA (health IDs), participate in the Health Records network, and share data through the HIE-CM gateway. Any
EMR operating in India that connects with government health schemes, insurance systems, or referral networks needs ABDM compliance. It’s not optional for 2025 and beyond.
-
Can an Indian EMR software company build for US healthcare clients?
Yes, but HIPAA compliance requires specific engineering practices: Business Associate Agreements (BAAs), documented security risk assessments, audit controls, access management, and encrypted data transmission and storage.
Several CMMI Level 5 companies in India have delivered HIPAA-compliant systems. Verify the vendor has done it before, not just claims to understand it.
-
What’s the difference between EMR, EHR, and HIS?
EMR (Electronic Medical Record) is a digital version of a patient’s chart within a single practice.
EHR (Electronic Health Record) extends across facilities and is designed for interoperability and sharing.
HIS (Hospital Information System) is the broader umbrella covering all hospital operations including billing, inventory, HR, and clinical systems.
Most large hospital builds are HIS projects that include an EMR/EHR as the clinical core.
-
How do you ensure data security in a cloud-based EMR?
A production-grade EMR should have: AES-256 encryption at rest, TLS 1.3 in transit, field-level encryption for sensitive identifiers, comprehensive audit logging, automated backup with tested recovery procedures, and regular penetration testing.
Data residency in India for ABDM compliance requires hosting in the India-region cloud infrastructure.