After reviewing the architecture of 40+ healthcare builds, I can tell you exactly where patient portal projects fall apart. It’s never the feature you’d expect.
And the stakes are higher than most teams realize, as per NIH, more than 3 in 4 individuals nationwide reported being offered online access to their medical records by their healthcare provider or insurer.
Patient portals are no longer optional infrastructure; they’re a default expectation.
It’s not the appointment scheduler. Not the lab results view. Not the billing module. It’s the integration layer — and every decision made before a single line of portal code gets written.
The EngineerBabu team has rebuilt more patient portals than we’ve built from scratch. Not because the original vendors couldn’t code. Because they scoped for features when they should have scoped for integrations, compliance architecture, and clinical workflows. Those are different projects with different failure modes.
Here’s what 14 years and 500+ product builds actually taught me about getting this right.
What Is a Patient Portal Development Company — and Why the Definition Matters
A healthcare development company builds software that gives patients direct digital access to their healthcare data, clinical interactions, and care management workflows. The operative word is “clinical.” This is not a booking widget. It’s not a telemedicine app with a FAQ section bolted on.
A properly built patient portal integrates with your EHR or HIS, pulls real-time clinical data through HL7 FHIR APIs, enables secure bidirectional messaging between patients and providers.
Moreover, it also supports e-prescriptions and lab result delivery, and does all of this inside a regulatory envelope that includes HIPAA, HITECH and 21st Century Cures Act interoperability mandates.
EngineerBabu is a CMMI Level 5 certified product engineering company that has delivered 500+ products across 20+ countries, including 75 YC-selected builds and 200+ VC-funded products.
Healthcare technology is one of our deepest verticals. I’m writing this because the information out there on patient portal development is, frankly, shallow — long on feature lists, short on what actually goes wrong.
The Real Scope of Patient Portal Development
Most buyers budget for features. They should be budgeting for integrations.
A patient portal is not a standalone application. It is an interface layer over existing clinical systems. The development effort is 30-40% UI/UX design and application logic, and 60-70% integration architecture, security infrastructure, and compliance instrumentation.
When a vendor gives you a quote without seeing your EHR environment, your data residency requirements, and your existing authentication systems — walk away.
Here’s what a full-scope patient portal actually covers:
Core Clinical Modules
- Patient demographics management and verified identity workflows
- Appointment scheduling with real-time calendar sync to your practice management system
- Lab results delivery with structured LOINC-coded data rendering
- Medication lists, refill requests, and e-prescription routing
- Secure patient-provider messaging with documented response SLAs
- Visit summaries and clinical notes (structured C-CDA documents)
- Immunization records, allergies, and care plan visibility
- Billing statements, EOBs, and online payment processing
- Proxy/caregiver access with delegated authorization controls
- Telehealth scheduling and video visit initiation
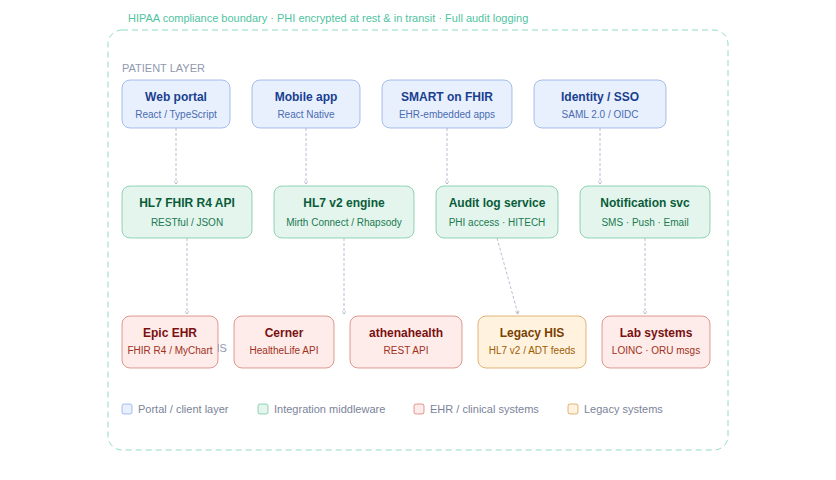
Integration Layer
This is where builds fail. Real interoperability requires:
- HL7 FHIR R4 API integration with your EHR (Epic, Cerner, Meditech, athenahealth, or custom)
- HL7 v2.x message translation for legacy systems still running on ADT feeds
- ICD-10 and SNOMED CT code mapping for clinical data normalization
- LOINC mapping for lab results
- Direct Protocol or SMTP-S for secure clinical messaging
- SSO integration with your identity provider (SAML 2.0 or OIDC)
- Payment gateway integration with HSA/FSA card support
Compliance and Security Infrastructure
- HIPAA-compliant data architecture with PHI encryption at rest and in transit
- Role-based access control (RBAC) with audit logging on every PHI access
- Business Associate Agreement (BAA) coverage across all infrastructure vendors
- HITECH breach notification workflow automation
- 21st Century Cures Act information-blocking compliance
- ONC Certified Health IT alignment where applicable
- Penetration testing and vulnerability disclosure program
How Much Does Patient Portal Development Cost?
I’ll give you the honest breakdown instead of the “it depends” non-answer.
| Build Scope | Timeline | Cost Range (USD) |
| MVP development — single EHR, core modules, web only | 4–6 months | $80,000–$150,000 |
| Mid-scale portal — multi-specialty, web + mobile | 6–10 months | $150,000–$350,000 |
| Enterprise portal — multi-site, full interoperability stack | 10–18 months | $350,000–$800,000+ |
| White-label SaaS portal platform | 12–24 months | $500,000–$1,500,000 |
These ranges assume a U.S. healthcare context with HIPAA compliance requirements. International builds in markets with different regulatory regimes (GDPR, UK NHS Digital standards, India’s DPDP Act) will vary in compliance architecture cost, not necessarily in feature cost.
What inflates cost beyond these estimates: legacy EHR systems with no FHIR support requiring custom HL7 v2 integration, multi-state deployments with state-specific consent law variations, biometric authentication requirements, and multi-language patient populations requiring clinical content localization.
What reduces cost: starting with a SMART on FHIR app framework rather than custom middleware, using a modular architecture that defers non-MVP modules to Phase 2, and engaging an engineering partner early enough to influence your EHR contract’s API access terms.

Patient Portal Architecture Decisions That Actually Matter
-
FHIR-Native vs. HL7 v2 Translation Layer
If your EHR supports FHIR R4 APIs, build natively against them. Don’t add a translation layer between FHIR and your portal data model — you’re adding latency, a failure point, and a maintenance burden you’ll carry for years.
If your EHR only exposes HL7 v2 interfaces (common in older Meditech, CPSI, or custom-built HIS environments), you need an integration engine — Mirth Connect, Rhapsody, or a cloud-native option like AWS HealthLake — as a middleware layer. Budget an additional 6-10 weeks of development and $15,000–$40,000 in integration engineering.
-
Microservices vs. Monolith
For single-facility, single-specialty implementations serving under 50,000 patient records, a well-structured monolith is defensible. It’s faster to build, cheaper to operate, and easier to audit.
For multi-site networks, health systems, or any deployment where patient volume will exceed 100,000 records within 3 years, microservices with event-driven architecture (Kafka or AWS EventBridge) is the correct call.
Appointment scheduling, messaging, lab results delivery, and billing each have different scaling profiles. They should not share a deployment unit or a database.
-
Cloud Infrastructure and HIPAA BAAs
Not all cloud configurations are HIPAA-compliant by default. You need a BAA in place with your cloud provider, and your architecture must be configured accordingly.
AWS HIPAA eligible services: EC2, RDS, S3 (with specific configurations), Lambda, EKS, and approximately 150 others. “AWS is HIPAA compliant” is incomplete — your architecture on AWS must be HIPAA-compliant.
The same logic applies to Azure and GCP. Database-level encryption, VPC isolation, CloudTrail-equivalent audit logging, and secrets management (not hardcoded credentials) are table stakes, not differentiators.
-
Authentication and Identity
Patient identity verification is a solved problem that vendors consistently under-implement.
At minimum: email verification + SMS OTP, with NIST AAL2 compliance for clinical data access. Better: identity proofing integration with Experian or LexisNexis for high-assurance identity (required if your portal surfaces controlled substance prescription history or behavioral health records).
For proxy access (parents accessing child records, adult children managing elder parent accounts), you need a delegated authorization model — not just shared credentials.
The EHR Integration Nobody Warns You About
I’ve worked with every major EHR vendor. Here’s the honest picture.
-
Epic MyChart vs. Custom Portal
If your health system runs Epic, the question isn’t whether to build a patient portal — it’s whether to build on top of Epic’s SMART on FHIR framework or build a separate portal with Epic FHIR API integration.
Epic’s own MyChart is deeply embedded in most health system contracts. Building a competing portal that integrates with Epic via FHIR APIs is possible but requires Epic to approve your SMART app registration, which takes 8–16 weeks and involves security review.
Custom portals built alongside Epic typically serve specialty-specific workflows that MyChart handles poorly — behavioral health, reproductive health, chronic condition management, or research participant portals where patient experience and branding control matter.
-
Cerner PowerChart
Cerner’s HealtheLife portal is less dominant than MyChart, making custom portal development more common in Cerner environments. Cerner’s FHIR APIs are generally more accessible for third-party developers. Budget 3–4 months for API access setup and sandbox testing regardless.
-
athenahealth
athenahealth’s API program is developer-friendly but has rate limits that bite hard at scale. If you’re building for a high-volume primary care network on athenahealth, design your caching layer and API call batching before writing a single line of portal UI code.
-
Custom/Legacy HIS
This is where builds get expensive. If your clinical system has no modern API development layer, you’re looking at an integration project that equals or exceeds the portal development effort in cost and timeline. I’ve seen organizations spend $120,000 on integration engineering for a portal that cost $180,000 to build.
What Most Patient Portal Development Companies Get Wrong
This is the part I can only write because I’ve seen it enough times.
-
They scope for features, not for workflows.
A patient viewing lab results is not a feature. It’s a workflow that includes: result delivery timing relative to provider review, abnormal result flagging, automatic patient notification, provider annotation visibility, and — critically — what happens when a patient sees a cancer marker without any clinical context.
Portal teams that think in features build portals that function but fail patients at their most vulnerable moments.
-
They treat compliance as a checklist.
HIPAA compliance is not a set of checkboxes. It’s an operational posture that must be designed into your data architecture from day one.
I’ve seen portals that “passed” a compliance review because the documentation was in order, while their audit logging was writing to a table with no retention policy, their PHI backups were unencrypted, and their API tokens were stored in environment variables on a shared staging server.
-
They don’t build for low health literacy.
The U.S. adult population has a median health literacy equivalent to a 7th-grade reading level. Most patient portals are written at a 12th-grade reading level. If your lab result says “Serum Creatinine 1.4 mg/dL (Reference Range: 0.7-1.2)” and you leave it there, you’ve delivered data, not information.
The best portals I’ve seen invest in content design as seriously as engineering — plain-language result summaries, contextual education modules, and escalation pathways for concerning findings.
-
They defer mobile to Phase 2 and never get there.
Patient portal adoption data is consistent: 60–70% of portal sessions happen on mobile devices. If your portal is not designed mobile-first from the start, you’re building a tool your patients won’t use.
“Mobile-responsive” is not mobile-first development. Responsive CSS on a desktop-designed application is not the same as a touch-optimized, performance-tuned, offline-capable mobile experience.
-
They underestimate the notification architecture.
Patients don’t check portals unprompted. Portal engagement is driven by notifications — new lab result, appointment reminder, message from provider, care gap alert.
The notification layer (push notifications for mobile, SMS, email) requires a separate microservice, integration with your clinical event bus, patient communication preference management, and opt-out workflows that comply with TCPA for SMS. This is 4–6 weeks of additional development that gets squeezed out of every first-time build.
Patient Portal Features vs. Patient Portal Capabilities: A Framework
Before evaluating vendors, separate features from capabilities. Any vendor can list features. Capabilities are what actually get used.
| Feature | The Capability That Matters |
| Appointment scheduling | Real-time slot confirmation + waitlist automation |
| Lab results | Contextual flagging + notification timing control |
| Secure messaging | Threaded conversation with SLA tracking + inbox management for providers |
| Prescription refills | Pharmacy routing + prior auth status visibility |
| Billing | EOB explanation + payment plan setup + HSA/FSA processing |
| Telehealth | Device-agnostic video with clinical document sharing during visit |
| Care plans | Editable goals + progress tracking + care team visibility |
Evaluate your vendor against the capability column, not the feature column.
How Long Does Patient Portal Development Actually Take?
I’ll break this down by phase, not by total timeline — because total timelines are meaningless without phase context.
Phase 1: Discovery and Architecture (4–8 weeks)
EHR environment audit, API access negotiation, data flow mapping, compliance architecture design, technology stack selection, integration design documentation. This phase is not optional and is not “consulting overhead.” Skipping it is how you end up rebuilding in month 6.
Phase 2: Core Infrastructure (6–10 weeks)
HIPAA-compliant infrastructure provisioning, authentication and identity layer, FHIR API integration scaffolding, audit logging framework, CI/CD pipeline with security scanning.
Phase 3: Feature Development — MVP Modules (10–16 weeks)
Patient demographics, appointment scheduling, lab results, secure messaging, medication management. These modules, done properly, take this long. If a vendor says 6 weeks for all of them, they’re building shallow.
Phase 4: Integration Testing and Compliance Validation (4–8 weeks)
EHR sandbox testing, penetration testing, HIPAA risk assessment, UAT with clinical staff and patient representatives, performance testing at projected load.
Phase 5: Rollout and Adoption (Ongoing)
Phased deployment by department or patient cohort, adoption analytics, feedback loop, iterative improvement.
Total for a production-ready MVP with real EHR integration: 6–9 months with a team that’s done it before. 9–14 months with a team doing it for the first time.
Choosing a Patient Portal Development Company: What to Actually Evaluate
Most RFP processes evaluate the wrong things. Here’s what to ask:
-
Can you show me a patient portal you’ve built, connected to an EHR, currently in production?
Not a prototype. Not a sandbox demo. Production. With real patients using it. If the answer involves NDAs that prevent any disclosure, that’s a signal — not a guarantee, but a signal.
-
Who will be on my project, and what is their healthcare software development experience?
Healthcare software development requires engineers who understand clinical workflows, not just software engineering. An engineer who’s built five fintech products may be excellent. They’re not automatically equipped for the regulatory and clinical complexity of healthcare.
-
How do you handle HIPAA subcontractor chain management?
Your portal will use cloud infrastructure, third-party APIs, analytics tools, communication services. Each of these is a potential Business Associate. A serious patient portal development company has a documented process for identifying, contracting, and monitoring their subcontractor BA chain. If they look confused by this question, stop the conversation.
-
What does your security incident response process look like?
Not “are you secure.” Not “do you have a SOC 2.” What happens in the first 4 hours after a detected breach? Who is notified? What is the chain of custody for forensic evidence?
HIPAA requires a documented incident response plan. Your vendor’s plan should be part of your contractual relationship.
-
How do you handle scope changes related to EHR upgrade cycles?
Epic, Cerner, and athenahealth release major API changes 1–2 times per year. If your EHR upgrades its FHIR implementation and your portal breaks, who is responsible and what does remediation look like? This should be in your contract, not your post-launch assumption.
If You’re Evaluating Patient Portal Development
I am usually the one on the early architecture calls. Not a sales team, not an account manager. If you’re trying to figure out whether what you need is a portal extension, a custom build, a SMART on FHIR app, or something else entirely — I’m happy to spend 30 minutes helping you think through it before you commit to anything.
Reach me at mayank@engineerbabu.com. Reference this article so I have context before we talk.
Mayank Pratap
Co-founder, EngineerBabu
14 years building technology products. 500+ projects delivered. Google AI Accelerator Top 20 (2024). CMMI Level 5.
FAQ: Patient Portal Development
-
What is the difference between a patient portal and a health app?
A patient portal has bidirectional connectivity to your clinical EHR system. It surfaces real clinical data — actual lab results, actual prescriptions, actual appointment history — in a regulatory-compliant environment.
A health app is a consumer wellness tool that may track symptoms or activity but does not integrate with your clinical record. The architectural complexity, compliance burden, and integration requirements are fundamentally different.
-
Does a patient portal have to be HIPAA compliant?
Yes, if it handles PHI (Protected Health Information) in the United States. A portal that displays actual patient records, lab results, medications, or appointment history is definitionally handling PHI.
HIPAA compliance requires technical safeguards (encryption, access controls, audit logging), administrative safeguards (policies, training, risk assessment), and physical safeguards for any hardware in scope. Cloud-hosted portals require BAAs with every service provider in the data chain.
-
How do patient portals integrate with EHR systems?
Modern EHR integration uses HL7 FHIR R4 APIs — RESTful APIs that return standardized clinical data in JSON format. Older EHR systems may require HL7 v2 interface engines that translate ADT, ORU, and SIU messages into portal-readable data structures.
Some EHRs support SMART on FHIR, a framework that allows third-party applications to launch within the EHR context with single sign-on and pre-authenticated patient context.
-
What is the typical patient portal development timeline?
For a production-ready portal with real EHR integration, single-facility deployment, and core clinical modules: 6–9 months with an experienced team. For enterprise multi-site deployments or platforms requiring white-label multi-tenancy, 12–18 months is realistic.
Timeline drivers are EHR API access complexity, compliance architecture requirements, and integration testing cycles — not feature development.
-
Can a patient portal be built on top of an existing EHR’s patient-facing interface?
Yes, in most modern EHR environments. Epic’s SMART on FHIR framework, Cerner’s app marketplace, and athenahealth’s API program all allow third-party portals to extend or replace the default patient-facing interface. The advantage is faster integration and SSO inheritance. The constraint is that you’re operating within the EHR vendor’s approval and certification process.