I recently sat down with the CTO of a mid-sized multi-specialty clinic chain. They had already spent ₹40 lakhs on a vendor, gone through two failed development cycles, and were back at zero — still running patient scheduling from a WhatsApp group and billing from spreadsheets.
The failure wasn’t a technology problem. It was a scoping problem that became a technology problem. They started building before they understood what they were actually building.
Clinic management software development is one of those projects where the gap between “we need software to run our clinic” and “here is what the system actually needs to do” is wider than most founders expect. I’ve seen it collapse teams, exhaust budgets, and set practices back by 18 months.
EngineerBabu, a CMMI Level 5 product engineering company, has built healthcare and fintech platforms across 20+ countries and 500+ projects. When we take on a clinic management system build, the first two weeks involve zero code. They’re all conversation, architecture whiteboarding, and compliance mapping. This guide reflects everything those conversations surface.
What Is Clinic Management Software Development?
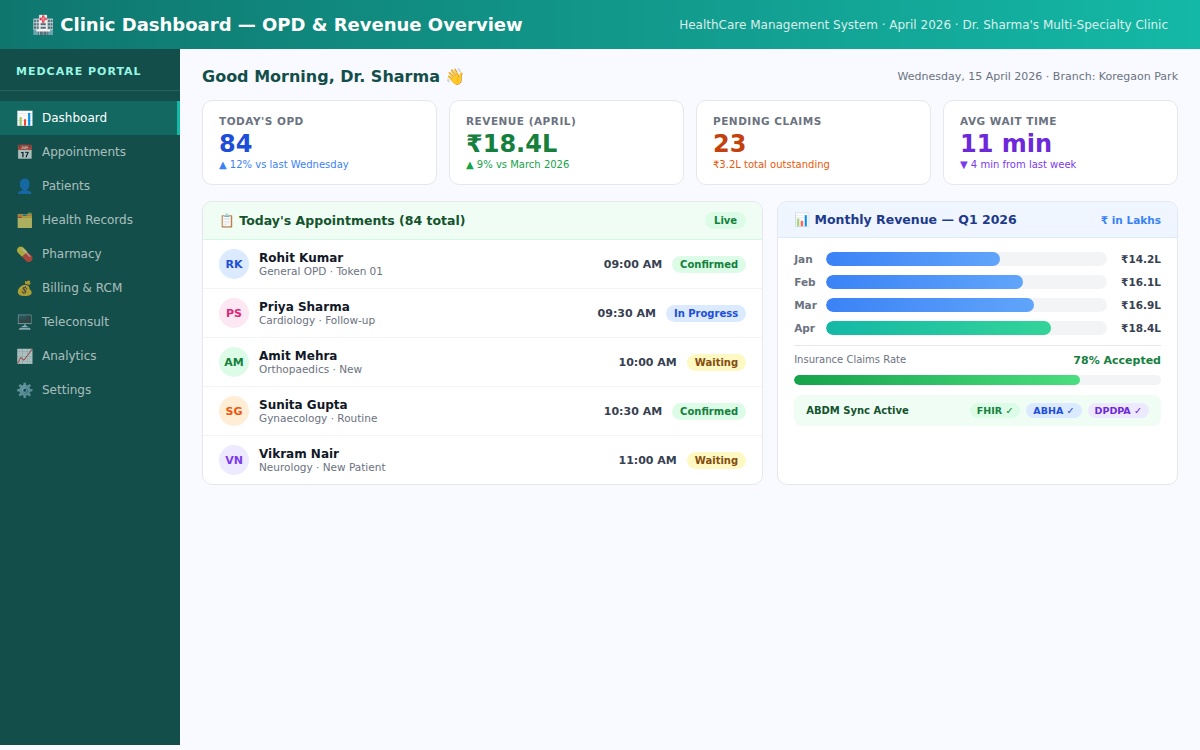
Clinic management software development is the process of designing, building, and deploying a digital platform that manages the operational, clinical, and financial workflows of a healthcare facility, including patient registration, appointment scheduling, electronic health records (EHR), billing, inventory management, staff management, and regulatory compliance within a single unified system.
The keyword here is “unified.” The problem with most off-the-shelf tools, and many custom builds, is that they solve one workflow while creating friction in three others.
The Scope Problem Most Clinics Underestimate
Most CTOs and clinic administrators I speak to underestimate the actual scope of a clinic management system by 3 to 4x. Not in features. In integrations.
A functioning clinic management platform in 2025 isn’t just a scheduling tool with a billing module bolted on. It needs to talk to insurance claim APIs, government health portals (in India, this means ABDM/ABHA integration), pharmacy management systems, diagnostic lab systems, payment gateways, SMS and WhatsApp notification services, and cloud storage for medical records — all with HIPAA-equivalent data privacy standards enforced at every layer.
According to a NASSCOM report, 63% of digital health implementation failures in India are attributed not to poor engineering but to incomplete requirement mapping at the pre-development stage.
If you go to a vendor with “we need an OPD management system,” you will get a price quote. What you won’t get is a question about whether you need multi-branch support, role-based access control across departments, offline-first functionality for locations with poor connectivity, or an audit trail that satisfies medical regulatory requirements.
Those questions need to come before the quote.
The Technical Architecture of a Clinic Management System
Core Modules You Cannot Cut
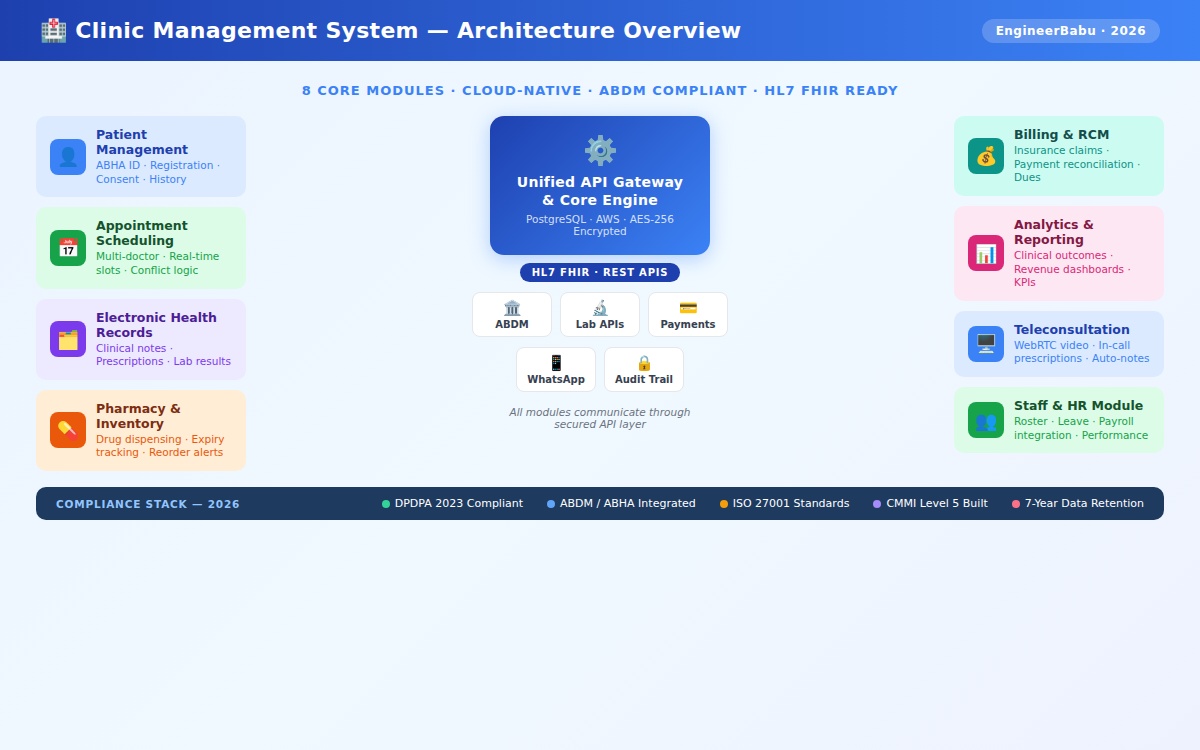
Before discussing architecture patterns, it’s worth being explicit about what a production-grade clinic management system actually contains. These are not optional:
- Patient Management Module: Registration, ABHA ID integration (in India), demographic data, patient history, consent management, and document storage. This module typically requires 6 to 8 weeks of engineering effort alone.
- Appointment Scheduling Engine: Multi-doctor, multi-branch, real-time slot management with conflict resolution logic. If you’re building for a specialty clinic with complex consultation workflows (pre-procedures, follow-ups, group bookings), this module gets complicated fast.
- Electronic Health Records (EHR): Structured clinical notes, prescription management, lab result integration, diagnostic imaging linkage. The data model here has to be designed carefully — retrofitting a poorly designed EHR schema costs more than building it right the first time.
- Revenue Cycle Management (RCM): Billing, insurance claim submission and tracking, payment reconciliation, outstanding dues management. For multi-specialty clinics, this module alone can take 3 to 4 months.
- Pharmacy and Inventory Management: Drug dispensing workflows, expiry tracking, reorder alerts, narcotic/scheduled drug compliance. Simba Beer, one of the companies the EngineerBabu team built inventory intelligence for, taught us that real-time inventory visibility with predictive restocking isn’t a “nice to have” — it’s operational infrastructure.
- Reporting and Analytics: Clinical outcomes dashboards, financial performance, occupancy rates, doctor productivity, patient retention metrics. Most clinics want this. Few include it in the initial scope.
- Staff and HR Module: Roster management, leave tracking, doctor performance records, payroll integration.
The Architecture Decision That Matters Most
Monolith or microservices — this is the first meaningful architecture call.
For a single-clinic setup processing under 200 OPD patients a day with one or two departments, a modular monolith deployed on a managed cloud service (AWS, GCP, or Azure) is faster to build, cheaper to maintain, and entirely sufficient.
For a multi-branch chain or a platform you intend to white-label for other clinics, microservices architecture with an API gateway, service mesh, and event-driven communication becomes the right call. The patient scheduling service, billing engine, and EHR system should be independently deployable.
I’d push back on anyone who recommends microservices to a 10-doctor single-location clinic. It adds 40 to 60% to your infrastructure complexity and doubles your DevOps overhead. The architecture should match the operational scale, not the engineer’s personal preference.
Technology Stack Decisions With Reasoning
- Backend: Node.js or Python (FastAPI or Django) for most clinic systems. Node works well for real-time scheduling and notification systems where concurrent connections matter. Python has stronger libraries for clinical data processing and any ML components (diagnostic assistance, appointment demand forecasting).
- Database: PostgreSQL as the primary relational store for structured clinical and billing data. It handles complex joins across patient, appointment, billing, and inventory tables far better than MongoDB in a clinical context. MongoDB is reasonable for unstructured notes and document storage as a secondary store.
- Frontend: React for web applications, React Native for cross-platform mobile (doctor and patient apps). For clinic administration interfaces that need rich scheduling views and complex forms, a well-architected React app outperforms alternatives.
- Cloud Infrastructure: AWS in India gives you the best combination of regional data residency compliance, managed database services (RDS), and healthcare-specific security controls. GCP is a strong second choice.
- ABDM Integration: If you’re building for the Indian market, Ayushman Bharat Digital Mission (ABDM) integration is not optional for new healthcare software. Plan for 4 to 6 weeks of integration and compliance work specifically for this.
Compliance Architecture: The Section Nobody Puts in Their Proposal
This is where most clinic management software proposals fail the clients who don’t know what to ask for.
Healthcare data is among the most regulated data in any jurisdiction. In India, the Digital Personal Data Protection Act (DPDPA) 2023, combined with ABDM compliance requirements and the Information Technology Act, creates a multi-layer compliance obligation that has to be designed into the architecture — not retrofitted.
- Data residency: Patient health data must reside on servers within India. This sounds obvious. It becomes complicated when your vendor uses a US-headquartered cloud provider without specifying the region.
- Encryption requirements: Data at rest and in transit with AES-256 minimum. Role-based access control with audit logs that cannot be modified by clinic staff.
- Consent management: Under DPDPA 2023, patients must be able to view, modify, and revoke consent for their data. This requires a consent management module that most template-based systems don’t have.
- Audit trails: Every record access, modification, and deletion needs a timestamped, user-attributed audit log. For regulatory scrutiny and medicolegal protection, this isn’t optional.
- Data retention: Medical records must be retained for a minimum of 7 years in most Indian states (some require longer for specific specialties). Your backup and archival architecture must reflect this.
Compliance cannot be a second-phase concern. Every architecture decision in phase one creates compliance debt or pays compliance investment.
Build vs. Buy vs. Customize: An Honest Framework
This is a decision most clinic founders make too quickly based on cost. The right answer depends on 4 variables.
| Factor | Buy Off-the-Shelf | Customize Existing Platform | Build Custom |
| Timeline | 4 to 8 weeks (deployment) | 3 to 5 months | 6 to 14 months |
| Cost (INR) | ₹2 to 8 lakhs/year subscription | ₹15 to 35 lakhs one-time | ₹30 to 80 lakhs+ |
| Customization | Low to medium | Medium to high | Complete control |
| Integration depth | Limited by vendor APIs | Moderate | Full flexibility |
| Scalability | Vendor-dependent | Partially controlled | Fully controlled |
| Long-term ownership | None | Partial | Complete |
| Best for | Single clinics, standard workflows | Multi-specialty, moderate custom needs | Multi-branch chains, platform ambitions |
The trap I see most often: a clinic chain with 8 branches buys an off-the-shelf tool to “start quickly,” hits customization ceilings within 6 months, and then commissions a full custom build anyway — having paid both costs.
If you have more than 3 branches, specific specialty workflows that standard tools don’t accommodate, or any ambition to operate as a technology platform, the custom build math works out better over a 3-year horizon.

What the Development Timeline Actually Looks Like
For a full-featured clinic management system with EHR, billing, scheduling, inventory, and ABDM integration, this is an honest timeline:
- Months 1 to 2: Discovery, architecture design, compliance mapping, UI/UX design
- Months 3 to 5: Core backend development — patient management, scheduling engine, EHR, authentication
- Months 5 to 7: Billing and RCM module, pharmacy/inventory module, ABDM integration
- Months 7 to 8: Reporting and analytics, staff management
- Months 8 to 9: Integration testing, security audit, compliance review
- Month 10: Pilot deployment with 1 to 2 locations, feedback loop
- Months 11 to 12: Full rollout, training, documentation
Most clinics hear “12 months” and try to negotiate it to 6. That negotiation usually results in a 14-month project that cuts testing time and compliance work. Don’t do that.
A lean version for a single-specialty clinic with basic EHR, scheduling, and billing (no pharmacy, no ABDM) can be done in 5 to 6 months. But you need to be specific about what you’re actually building.
Key Features That Determine Platform Quality
-
Patient Portal and Engagement Layer
A patient portal isn’t just an appointment booking screen. It’s the clinic’s relationship infrastructure. Online appointment booking, prescription history access, lab result viewing, teleconsultation integration, payment history, and discharge summary download should all be part of a production patient portal.
The platforms that do this well see 25 to 35% reduction in front-desk call volume within 90 days of launch.
-
Teleconsultation Integration
Post-pandemic, teleconsultation is a standard clinical offering, not a feature differentiator. WebRTC-based video consultation with in-call prescription writing, secure document sharing, and automatic consultation notes saved to the patient EHR is now table-stakes for a 2025 clinic management platform.
-
Clinical Decision Support (CDS)
This is where AI enters the picture meaningfully. Drug interaction checks at the point of prescription, dosage alerts based on patient weight and age, allergy flag integration, and diagnosis code suggestions (ICD-10/ICD-11) are CDS features that reduce clinical risk and have measurable impact on prescribing accuracy.
These aren’t AI marketing. They’re rules-based and ML-augmented systems that require careful design but deliver real clinical value.
-
Interoperability
HL7 FHIR standard compliance is the architecture direction for healthcare data exchange globally. If your system can’t speak FHIR, it can’t integrate with national health exchanges, external diagnostic labs, or specialist referral networks without custom API work every single time. Build to FHIR from the start.
Real Cost Breakdown for Clinic Management Software Development
These are real ranges based on projects the EngineerBabu team has delivered:
- Basic system (single clinic, scheduling + billing + basic EHR, no ABDM):
₹18 to 28 lakhs, 4 to 5 months - Mid-range system (2 to 5 branches, full EHR, pharmacy, ABDM integration, patient portal):
₹35 to 55 lakhs, 7 to 9 months - Enterprise platform (multi-branch chain, white-label potential, full compliance architecture, analytics, teleconsultation):
₹65 to 1.2 crores, 10 to 14 months - Annual maintenance and hosting (post-launch):
15 to 20% of development cost per year
Note: These figures assume a competent product engineering team, not the cheapest-quote freelancer market. The ₹8 lakh clinic management system quote you’ll find on Upwork will cost you ₹30 lakhs to fix.
How to Evaluate a Development Partner
Before signing any clinic management software development contract, ask these specific questions:
- Have you built and deployed an EHR system before? Can I speak to the client?
- Who handles ABDM integration — an in-house healthcare specialist or a subcontractor?
- What’s your compliance review process? Do you have a security audit step?
- How do you handle the offline-first requirement for low-connectivity locations?
- What does the post-launch support contract look like? What’s included vs. billable?
- Who owns the codebase and data post-delivery?
A vendor who can answer all 6 questions with specificity is worth talking to further. A vendor who deflects, generalizes, or schedules a “follow-up call” for half of them probably hasn’t done this before.
If You’re Evaluating Clinic Management Software Development Right Now
The architecture decisions you make in the first 4 weeks determine the operational ceiling of your platform for the next 5 years. I’ve seen that compression cost clinics ₹60 lakhs in rebuild work that could have been ₹8 lakhs in design time upfront.
If you’re at the stage of evaluating vendors, defining scope, or questioning whether to build or buy — I’m usually the one on those architecture calls personally.
Mayank Pratap
Co-founder, EngineerBabu
14 years building technology products. CMMI Level 5 certified. Google AI Accelerator — Top 20 globally, 2024. Backed by Vijay Shekhar Sharma. 500+ products delivered across 20+ countries, including 75 YC-selected builds and 4 unicorn clients.
EngineerBabu takes 20 projects per year. Every client comes from referral. No sales team.
FAQ
-
How long does it take to build clinic management software?
A basic single-clinic system with scheduling, billing, and EHR takes 4 to 6 months. A full multi-branch enterprise platform with ABDM integration, analytics, pharmacy, and teleconsultation typically takes 10 to 14 months. Compressed timelines without cutting scope usually mean cutting testing, compliance review, or both — which creates problems within 6 months of launch.
-
What is the cost of developing a custom clinic management system in India?
Costs range from ₹18 to 28 lakhs for a basic single-clinic setup to ₹65 lakhs to 1.2 crores for an enterprise-grade multi-branch platform with full compliance architecture. The actual cost depends on module scope, number of integrations, compliance requirements, and the experience level of the development team.
-
Is ABDM integration mandatory for clinic management software in India?
ABDM integration is not currently legally mandatory for all private clinics, but it is increasingly required for participation in government health schemes, insurance claim processing, and national health record portability. For any clinic management system built in 2025, ABDM integration should be treated as a non-negotiable architecture requirement, not an optional module.
-
What database should be used for clinic management software?
PostgreSQL is the recommended primary database for clinic management systems. It handles complex relational queries across patient, appointment, billing, and inventory data with strong ACID compliance and native support for JSON when you need flexible document storage. MongoDB can serve as a secondary store for unstructured clinical notes, but using it as the primary database for a healthcare platform introduces data integrity risks.
-
Can clinic management software be built on a SaaS model?
Yes, and it’s often the right architecture for clinic chains or anyone building a product they intend to license. A SaaS clinic management platform requires multi-tenancy architecture, data isolation between clinic clients, subscription billing integration, and role-based onboarding flows. The development investment is 40 to 60% higher than a single-tenant build, but the revenue model supports it if your target market is other clinics.




