I recently had a call with a healthtech founder who had already spent $180,000 on a medical billing platform. The product had been “done” twice. Neither version ever went live. When I asked him what went wrong, he said the same thing I hear constantly: “We didn’t realize how complicated the payer side was.”
He wasn’t wrong. But it wasn’t the payer complexity that sank the project. It was that nobody on his team had mapped the compliance requirements before they wrote a single line of code. HIPAA. ICD-10. HL7 FHIR. 837P and 835 transaction sets. They found out about each one after the architecture was already locked.
I’ve been building technology products for 14 years. The EngineerBabu team has delivered 500+ projects across 20+ countries, including some of the more complex fintech stacks in India. When a healthtech client approached us to build a full revenue cycle management system, the first two weeks were entirely research and compliance mapping. No code. That decision saved the client roughly six months of rework later.
This article is what I wish someone had handed that founder before he signed his first development contract.
What Is Medical Billing Software Development?
Medical billing software development is the process of designing, building, and deploying systems that handle the end-to-end revenue cycle for healthcare providers. This includes patient registration, insurance eligibility verification, charge capture, claim generation (837P/837I transaction formats), clearinghouse submission, remittance processing (835 files), denial management, and patient payment collection.
The scope is almost always larger than clients initially estimate. A “billing module” sounds like a single feature. In practice it’s 7 to 12 interconnected subsystems, each with its own compliance requirements, third-party integrations, and data security obligations.
According to the National Institute of Health, healthcare administrative transactions — largely claims processing — cost the US healthcare system $12 to $19 per claim. That efficiency gap is exactly where purpose-built billing software creates value.
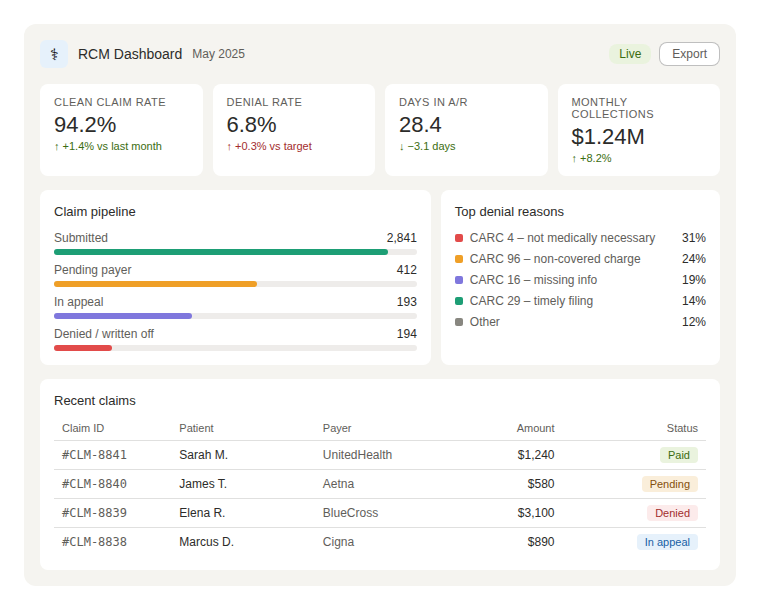
The Real Cost of Medical Billing Software Development
This is the question every client asks first, and the answer almost no one gives honestly.
Most “cost guides” online will tell you $50,000 to $500,000 and call it a range. That’s not useful. Let me break it down by system scope.
-
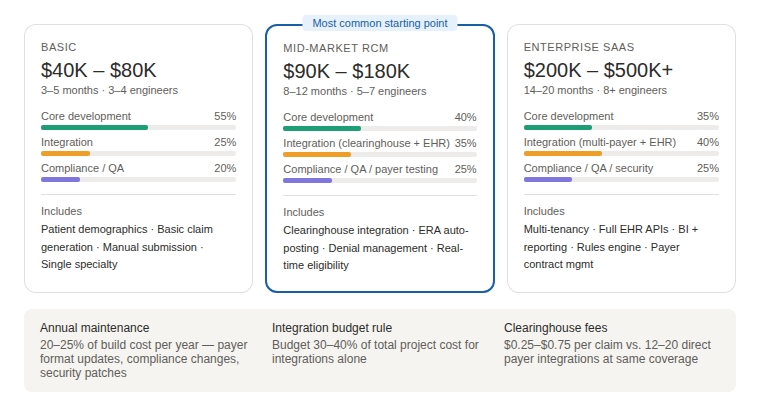
Basic practice management with billing module: $40,000 to $80,000
This covers patient demographics, scheduling, basic claim generation, and manual submission. No real-time eligibility verification. No ERA/EFT automation. No clearinghouse integration. Useful for a single-specialty small practice, not scalable.
-
Mid-market RCM platform: $90,000 to $180,000
Adds clearinghouse integration (Availity, Change Healthcare, or Waystar), automated eligibility verification, claim status tracking, basic denial management workflow, and remittance posting. This is where most startup projects should start if they’re building for multi-provider practices.
-
Enterprise medical billing system: $200,000 to $500,000+
Full revenue cycle management. Multi-tenant architecture. Payer contract management. Predictive denial prevention. Business intelligence and reporting. Custom rules engine for charge capture. Integration with major EHR systems (Epic, Cerner, Athena). If you’re building a billing SaaS product to sell to hospital networks, this is the range.
These numbers assume a competent development team working full-time. They don’t account for ongoing maintenance, which typically runs 20 to 25% of initial build cost annually.
The thing most CTOs I talk to underestimate is integration cost. Budget 30 to 40% of your total development budget for integrations alone. EHR APIs, clearinghouses, payer portals, payment processors, and credit bureaus are not plug-and-play.
They’re negotiated relationships, and each one has its own data format, authentication protocol, and test environment.
HIPAA Compliance in Medical Billing Software: What Actually Matters
Almost every article on this topic lists the HIPAA rules and calls it done. That’s not engineering guidance. Let me tell you what it actually means to build HIPAA-compliant software.
-
Protected Health Information (PHI) scope is wider than you think
Patient names, dates of service, diagnosis codes, claim amounts, even IP addresses tied to patient records are all PHI. Your encryption strategy, access control model, and audit logging architecture need to be designed around PHI from day one. Not retrofitted.
-
Technical safeguards you can’t skip
Encryption at rest (AES-256 minimum) and in transit (TLS 1.2 or higher). Role-based access control with the principle of least privilege. Audit logs for every PHI access and modification. These need to be immutable. Automatic session timeouts. Multi-factor authentication for all administrative access.
-
Business Associate Agreements (BAAs)
Every third-party service that touches PHI needs a BAA. Your cloud provider (AWS, GCP, Azure all offer HIPAA-eligible services). Your clearinghouse. Your analytics platform. I’ve seen projects delayed three to four months because someone tried to plug in a standard BI tool mid-development without realizing it didn’t offer BAAs.
-
The 2025 enforcement reality
HHS OCR settlements for HIPAA violations reached record levels in 2024, with the average settlement for a mid-size provider breach running $1.2 million. Building compliance in from architecture is 10x cheaper than a post-breach remediation.
Core Modules: How to Architect a Medical Billing System
This is the technical section competitors skip. They list features. I’m going to walk you through the architecture decisions that actually matter.
-
Patient Registration and Eligibility Verification
The entry point for every billing workflow. Eligibility verification needs to happen in real time before the appointment, not after the claim is denied. This requires direct API integration with payer portals or a clearinghouse that provides 270/271 transaction handling.
Design this as an async service with retry logic. Payer APIs fail at surprisingly high rates. A synchronous call that blocks patient check-in for 30 seconds because United Healthcare’s API is slow is a UX disaster. Queue the verification, cache the result with a TTL of 24 hours, and surface a fallback UI.
-
Charge Capture and Coding
Charge capture is where CPT codes, ICD-10 diagnosis codes, and modifiers are assigned to services rendered. This is where clinical and billing intersect. The most common integration point is with your EHR (HL7 FHIR R4 is now the standard), but for standalone billing software you’ll often need to build a manual charge entry interface with code lookup and validation.
Build a rules engine here. Clinical logic like “procedure code 99213 requires a diagnosis from these ICD-10 categories” can prevent thousands of unnecessary claim rejections. Most teams build this as a static table. That’s fine for version one. In version two you’ll want a configurable, client-managed rules layer.
-
Claim Generation and Clearinghouse Submission
The 837P (professional) and 837I (institutional) transaction formats are the backbone of claim submission in the United States. These are X12 EDI documents with specific segment structures, loop hierarchies, and element codes that payer systems parse.
Don’t build an X12 generator from scratch. Use a tested library (PHPEdi, Stedi, or similar). The risk isn’t the format itself. The risk is payer-specific requirements on top of the standard. Certain payers require custom NPI taxonomies, specific claim frequency codes, or proprietary loop extensions. Test against each payer’s sandbox individually.
Clearinghouse integration is almost always the right call over direct payer submission for anything beyond a single large health system. Availity, Waystar, and Change Healthcare each cover 95%+ of commercial payer volume.
The tradeoff is clearinghouse fees (roughly $0.25 to $0.75 per claim) versus direct payer integration complexity (12 to 20 separate payer API integrations to reach the same coverage).
-
ERA and EFT Automation
Electronic Remittance Advice (835 files) is how payers tell you what they paid and why. Electronic Funds Transfer is how they actually pay. Automating the reconciliation of 835 remittance data against your claim records is where billing software creates immediate ROI.
This module needs to handle partial payments, contractual adjustments, recoupments, and denial reason codes. Build a parser for the 835 file format that maps CARC/RARC codes to actionable workflow steps. A denial for CARC 4 (the service is inconsistent with the patient’s history) should automatically route to a clinical review queue. A denial for CARC 96 (non-covered charge) should trigger a patient billing workflow.
-
Denial Management
This is the module most underinvested in early-stage products. Denial rates industry-wide run 5 to 10% of submitted claims. In a $5M revenue practice, that’s $250,000 to $500,000 at risk. A proper denial management workflow tracks denial reason, calculates appeal deadlines by payer, routes to the right staff role, and tracks resolution.
Build this with a state machine, not a status field. “Denied” is not a state. “Denied, eligible for appeal, appeal due in 30 days, assigned to coder review” is a state. The difference is whether you recover the revenue or write it off.
Technology Stack Decisions (With My Actual Opinions)
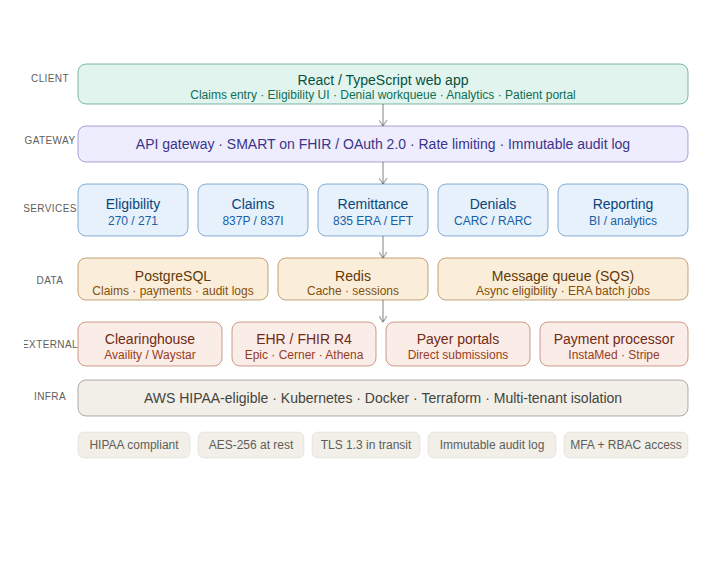
- Backend: Node.js or Python (FastAPI) for API services. Both handle the async patterns you need for integration-heavy billing systems. I’d pick Python for anything with heavy data processing (835 parsing, reporting aggregation). Node for the real-time eligibility and claims-status services.
- Database: PostgreSQL for transactional data. Every claim, every payment, every audit log. Don’t use MongoDB for this. Billing data is highly relational, and you’ll run analytics queries that rely on JOINs your document store will make painful. Use Redis for session management and eligibility result caching.
- HL7 FHIR: If you’re integrating with EHRs, build to FHIR R4. The SMART on FHIR authorization model is how you’ll authenticate against Epic and Cerner production environments. Plan for this from the start. Retrofitting FHIR onto a non-FHIR architecture is a full rewrite.
- Architecture pattern: Microservices for anything you’re building at scale. Single service per bounded context: eligibility, claims, remittance, patient billing, reporting. Each service owns its data. Deploy on Kubernetes if you’re serious about multi-tenant SaaS. This gives you the isolation you need for HIPAA-compliant tenant separation.
- Cloud provider: AWS GovCloud or AWS standard with HIPAA-eligible services configuration. Both Azure and GCP have equivalent offerings. AWS has the deepest ecosystem of healthcare-specific tooling (Amazon HealthLake, etc.) but choose based on your team’s expertise, not marketing.
Timeline Reality: How Long Does This Actually Take?
I’ll give you the ranges based on what I’ve actually seen, not what vendors quote to win the deal.
- Basic practice billing module: 3 to 5 months with a team of 3 to 4 engineers. This assumes no custom reporting, limited payer integration (one clearinghouse), and no mobile.
- Mid-market RCM platform: 8 to 12 months with a team of 5 to 7. The long tail is always integration testing against payer sandboxes. Each payer environment is different. Build 6 to 8 weeks of integration QA into your plan.
- Enterprise medical billing SaaS: 14 to 20 months for v1 production. This is the “we’re building a company around this” scope. Plan for a phased launch: subset of payers, subset of specialties, single-tenant first.
- The biggest schedule killers I’ve seen repeatedly: HIPAA security assessment not started early enough, clearinghouse credentialing delays (4 to 8 weeks for production access), and underestimating the time to build reliable test data.
What Most People Get Wrong About Medical Billing Software
I’ve reviewed the architecture of at least 12 billing platforms in the last 3 years. Here is the pattern I see in the ones that fail.
- They build a billing interface, not a billing system. A nice UI for entering claims is not a billing system. A billing system has automation rules, exception queues, denial tracking, payer-specific logic, and reporting that tells you where revenue is leaking before the practice manager notices. The UI is 20% of the work.
- They underinvest in the remittance layer. ERA automation is unsexy. Parsing 835 files is not the kind of work that gets in demos. But it’s where real ROI lives. If your system doesn’t automate posting and denial routing, billing staff are still doing manual work and you haven’t actually replaced the problem.
- They design single-tenant from the start. If you’re building a SaaS product, multi-tenancy needs to be in the data model from day one. Row-level security in PostgreSQL, tenant isolation in your API gateway, separate encryption keys per tenant. Retrofitting multi-tenancy into a single-tenant schema after launch is one of the most painful technical migrations I’ve seen.
- They treat HIPAA as a checklist, not a design constraint. HIPAA compliance isn’t a module you add. It’s a set of constraints that shapes your entire architecture. Teams that approach it as a post-launch checklist end up rebuilding their access control model, their logging infrastructure, and their data encryption strategy. That’s $40,000 to $80,000 of rework that a proper upfront design review would have prevented.
Build vs. Buy: When Does Custom Development Make Sense?
There are excellent off-the-shelf billing systems: Kareo, AdvancedMD, DrChrono, Waystar’s practice management tools. For a standard single-specialty practice that wants to start billing tomorrow, a SaaS billing platform is almost always the right answer.
Custom development makes sense when:
The business model requires white-labeling. You’re building a billing SaaS to resell, not consuming one.
The specialty has unusual billing logic. Behavioral health, home health, durable medical equipment, and long-term care all have claim structures and compliance requirements that standard platforms handle poorly.
You need deep EHR integration. A custom billing engine that sits inside your proprietary EHR or care management platform needs to be built, not bolted on.
You’re building for scale. If you’re processing 100,000+ claims per month across 500+ providers, the per-claim fees on SaaS platforms become a significant cost line. Custom infrastructure at scale often beats SaaS unit economics above a certain volume threshold.
| Factor | Use SaaS | Build Custom |
| Time to launch | Weeks | 6 to 18 months |
| Upfront cost | Low ($500/mo to $5K/mo) | $80K to $500K |
| Scale economics | Higher per-claim cost | Lower at volume |
| Specialty complexity | Standard specialties | Complex/unusual billing |
| White-label needs | Not possible | Core use case |
| EHR integration depth | Limited | Full control |
What the EngineerBabu Team Has Learned Building Complex Healthcare Systems
When we built the lending stack for EarlySalary, now processing over ₹10,000 crore in disbursements, the core lesson was the same one that applies to healthcare: compliance and integration are not features you add. They’re constraints that shape every architectural decision from database schema to deployment model.
The teams that ship successful medical billing systems share a few traits. They map the compliance requirements before the first sprint. They budget honestly for integration complexity. They build the boring parts (remittance automation, denial tracking, audit logging) with the same care as the visible features. And they test against real payer environments, not just their own mocks.
The teams that fail ship a beautiful claims entry interface, discover that their architecture can’t handle ERA automation without a rebuild, realize they forgot to design for multi-tenancy, and run out of money before they ever go live.
You don’t have to repeat those mistakes.
Ready to Evaluate Your Medical Billing Software Architecture?
If you’re planning a medical billing software development project and want to talk through the architecture decisions before you commit to a team or a scope, I’m the one on those calls at EngineerBabu.
We take 20 projects a year. Every client comes from referral. If this article gave you useful signal, that’s already a better conversation than most vendor introductions.
Mayank Pratap Co-founder, EngineerBabu 14 years building technology products. Google AI Accelerator Top 20 (2024). CMMI Level 5 certified. 500+ projects across 20+ countries. Harvard Innovation Labs participant.
EngineerBabu is a CMMI Level 5 certified product engineering company. We’ve built 200+ VC-funded products, including 75 YC-selected products and 4 unicorn-backed platforms.
Medical Billing Software Development: Frequently Asked Questions
-
How long does it take to build a medical billing system from scratch?
For a functional mid-market platform with clearinghouse integration, eligibility verification, and denial management, plan for 8 to 12 months. Simple practice billing modules can be built in 3 to 5 months. Enterprise RCM systems with full EHR integration and multi-tenancy run 14 to 20 months. The long tail is almost always integration testing, not feature development.
-
What are the HIPAA requirements for medical billing software?
Technical safeguards include AES-256 encryption at rest and TLS 1.2+ in transit, role-based access control, immutable audit logs covering all PHI access, automatic session timeouts, and MFA for administrative users. All third-party services touching PHI require signed Business Associate Agreements. Your cloud infrastructure must use HIPAA-eligible service configurations.
-
How much does medical billing software development cost?
Basic billing modules start at $40,000 to $80,000. Mid-market RCM platforms run $90,000 to $180,000. Enterprise systems range from $200,000 to $500,000+. Budget 30 to 40% of total cost for integrations (clearinghouses, EHRs, payer portals, payment processors), and 20 to 25% annually for ongoing maintenance.
-
What integrations does medical billing software need?
At minimum: one clearinghouse (Availity, Waystar, or Change Healthcare) for claim submission and remittance. Real-time eligibility verification (270/271 transactions). A payment processor (Stripe, Square, or healthcare-specific like InstaMed). If clinical data is involved, an EHR integration via HL7 FHIR R4. Larger systems add payer portals for appeals, credit bureau reporting for collections, and BI tools for analytics.
-
What is the difference between 837P and 837I claims?
837P is the professional claim format used by individual physicians and outpatient facilities. 837I is the institutional claim format used by hospitals and inpatient facilities. Both are X12 EDI transaction sets, but they have different loops, segments, and data requirements. Your claim generation module needs to support both if you’re building for mixed provider types.




