Three months into building a remote patient monitoring platform, a health-tech founder walked me through their architecture with one burning complaint: Bluetooth vitals data arriving 4-6 seconds late. Not a disaster in isolation.
Except their system was triggering alerts 4-6 seconds after the threshold breach — and for a cardiac monitoring use case, that gap isn’t a latency issue, it’s a liability.
They had hired a solid engineering team. The app looked excellent. The backend was clean. The problem was that nobody had made a conscious architectural decision about real-time data pipelines early enough, so the system was built on request-response patterns instead of event-driven streaming. Fixing it required rebuilding 40% of the backend.
I’ve seen this exact mistake, in different forms, across 15+ health tech builds at EngineerBabu — a CMMI Level 5 certified product engineering company that has shipped 200+ VC-funded products across 20+ countries.
The mistake is never the feature you’d expect. It’s always an architectural assumption that seemed reasonable at month one and became expensive at month four.
This guide is what I tell founders before they write a single line of remote patient monitoring code.
What Is Remote Patient Monitoring App Development?
Remote patient monitoring (RPM) app development is the process of building software systems that continuously collect, transmit, analyze, and act on patient health data from outside clinical settings — typically from wearable devices, home monitoring equipment, or mobile applications connected to biosensors.
The word “continuously” is doing a lot of work in that sentence. An RPM system isn’t an online consultation app with video calls. It’s a real-time data infrastructure that happens to have a clinical interface on top. That distinction matters enormously for every architectural decision you’ll make.
The global RPM market was valued at $27.72 billion in 2024 and is projected to reach $59+ billion by 2026 according to MarketsandMarkets research. The demand is real. The execution complexity is significantly underestimated.
The Core Architecture Decision Nobody Talks About
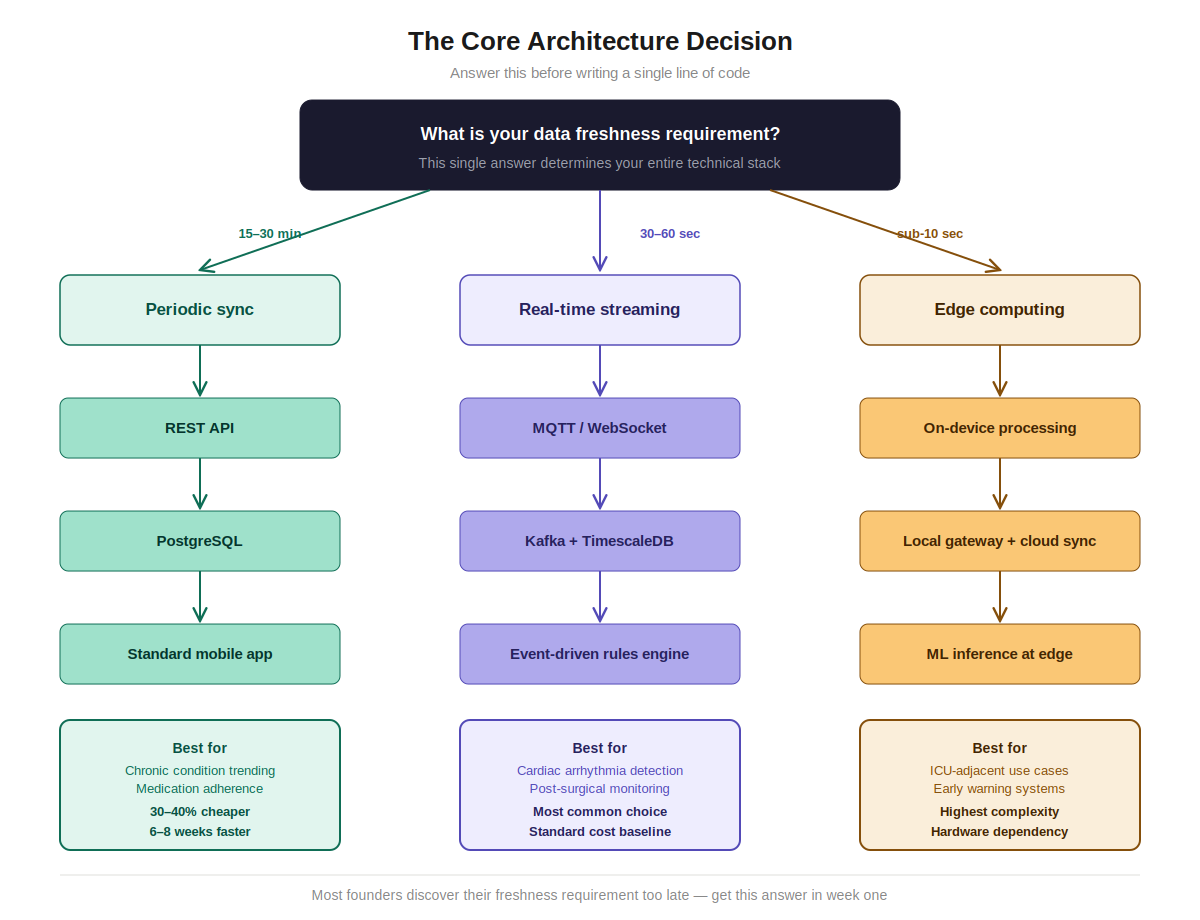
Before you think about features, you need to answer one question: what is your data freshness requirement?
This question determines your entire technical stack.
- If your clinical use case tolerates 15-30 minute data windows — think post-discharge medication adherence or chronic condition trending — you can build on a standard REST API architecture with periodic sync. Lower complexity, lower cost, faster to ship.
- If your use case requires alerts within 30-60 seconds — think cardiac arrhythmia detection, hypertension management, post-surgical monitoring — you need real-time event streaming. WebSockets or MQTT for device-to-cloud communication, Apache Kafka or AWS Kinesis for data ingestion, stream processing for rule evaluation before data hits your database.
- If your use case requires sub-10-second response — ICU-adjacent monitoring, early warning systems — you’re in edge computing territory. Processing needs to happen on the device or local gateway, not round-tripped through the cloud.
The EngineerBabu team has built all three. The cost and timeline differences are not incremental — they’re multiplicative. A periodic-sync RPM MVP development typically costs 30-40% less and ships 6-8 weeks faster than an equivalent real-time streaming architecture.
Most founders discover their freshness requirement late. Don’t let that be you.
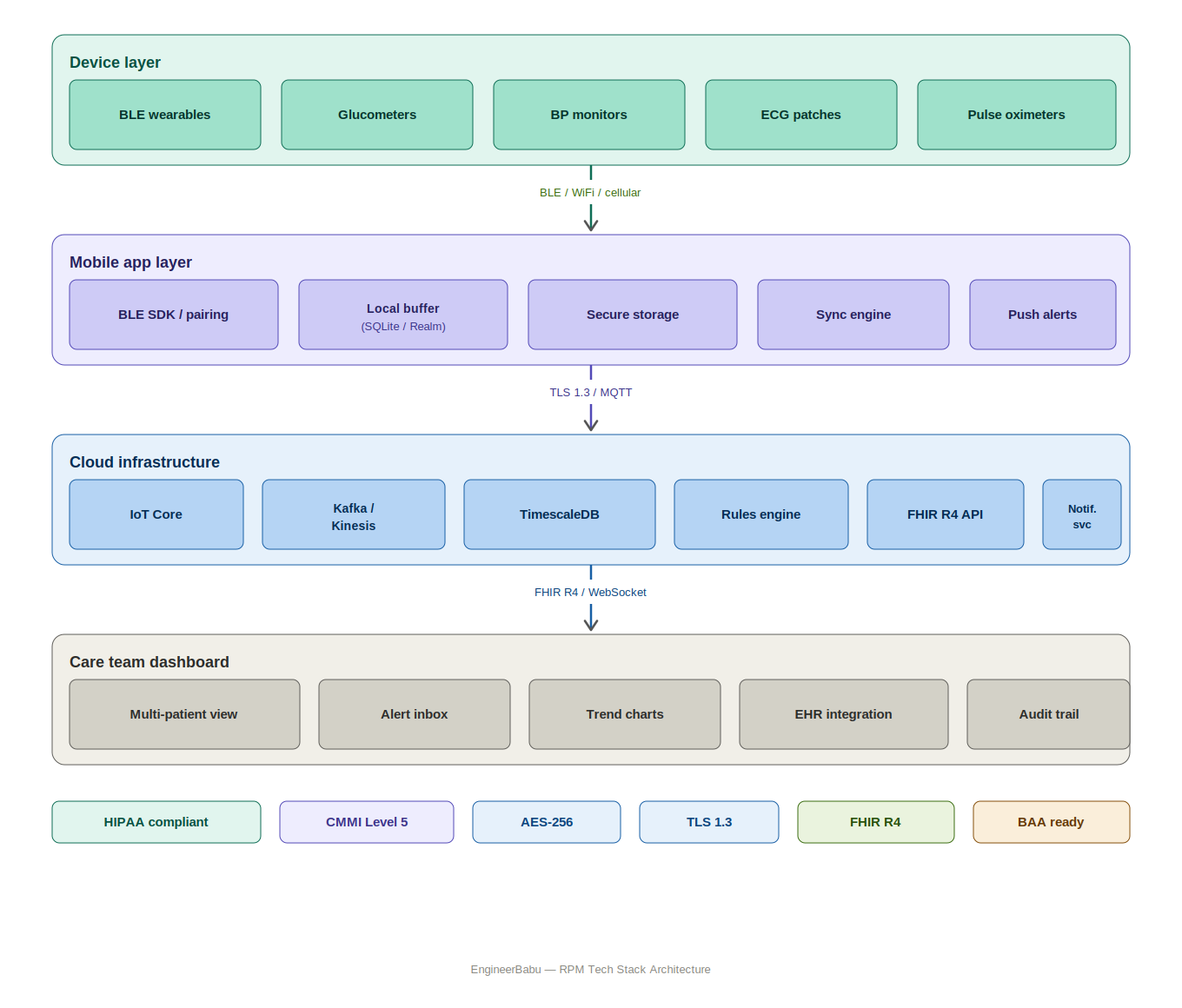
Remote Patient Monitoring App Development: The Full Tech Stack
-
Device Layer: Where Most Projects Underestimate Complexity
Wearable devices and biosensors communicate through a mix of Bluetooth Low Energy (BLE), Zigbee, cellular (CAT-M1/NB-IoT), and WiFi. Each has different range, power consumption, and reliability characteristics.
BLE is the most common for consumer wearables. The problem with BLE in clinical contexts is connection stability. A patient moves away from their phone, the connection drops, data is lost. Your system needs to handle this gracefully — local buffering on the device, re-sync on reconnect, gap detection in your data quality layer.
The device integration layer typically involves:
- A BLE/sensor SDK for the specific hardware you’re integrating (Polar, Withings, Garmin, Dexcom, iHealth, and others all have different SDKs)
- A custom native mobile app or a React Native/Flutter wrapper with BLE libraries (react-native-ble-plx for React Native, flutter_blue_plus for Flutter)
- Device pairing flow, authentication, and firmware version management
- Local data buffering for offline scenarios
- Battery and signal strength monitoring
One thing I tell every RPM team: budget a dedicated 3-4 week sprint just for device integration work. Not alongside other feature development — dedicated. The hardware edge cases will eat your timeline if you fold device integration into general sprint work.
-
Mobile App Layer
The mobile app in an RPM system has a different purpose than most consumer health apps. It’s less about engagement and more about reliability as a data conduit.
Your patients are often elderly, managing chronic conditions, not necessarily tech-native. The UI needs to be simple to the point of being obvious. But the engineering underneath needs to handle:
- Background data collection — iOS background mode restrictions are brutal. Apple restricts background BLE activity in ways that can interrupt continuous monitoring. This requires a specific entitlement (com.apple.developer.bluetooth.background-modes) and careful management of background task time.
- Local SQLite or Realm database for offline buffering
- Push notification handling for patient alerts and care team communications
- Secure local storage for PHI — using iOS Keychain or Android Keystore, not AsyncStorage or SharedPreferences
On framework choice: I’d recommend React Native if you have a tight budget and a single team that needs to ship both platforms simultaneously. But if your use case involves intensive BLE processing or you’re building for a patient population where iOS performance matters critically, native Swift/Kotlin is worth the additional cost.
-
Cloud Infrastructure Layer
This is where RPM differs most dramatically from standard health apps.
A typical RPM cloud backend needs:
- IoT ingestion layer — AWS IoT Core, Azure IoT Hub, or Google Cloud IoT for managing device connectivity and certificate-based authentication
- Message queue / stream processor — Apache Kafka, AWS Kinesis, or RabbitMQ depending on volume and latency requirements
- Time-series database — TimescaleDB (PostgreSQL extension), InfluxDB, or AWS Timestream for storing sequential vitals data efficiently. Standard relational databases handle time-series data poorly at scale
- Rules engine — clinical alert logic, threshold evaluation, escalation workflows
- FHIR-compliant API layer — HL7 FHIR R4 is increasingly the interoperability standard, especially if you need EHR integration
- Notification service — multi-channel (push, SMS, email, pager) for care team and patient alerts
On cloud vendor: AWS has the most mature IoT and healthcare ecosystem. Azure is strong if your hospital clients are Microsoft shops (many are). GCP is solid for ML-heavy use cases. Most RPM platforms I’ve seen end up on AWS.
-
Care Team Dashboard
The clinician-facing web dashboard has different UX requirements than consumer apps. Care team members are monitoring multiple patients simultaneously, triaging alerts, and documenting interventions.
Key dashboard features that matter clinically:
- Multi-patient vitals overview with alert prioritization
- Time-series data visualization (trend charts, not just snapshots)
- Alert inbox with acknowledgment and escalation workflows
- Care plan and threshold customization per patient
- EHR integration for notes documentation
- Audit trail for every clinical interaction
I’ve seen many teams build patient-facing apps well but build clinician dashboards like they’re designing a consumer product. Clinicians don’t want beautiful. They want fast, accurate, and auditable.
HIPAA Compliance in RPM App Development: The Non-Negotiables
Every RPM system that handles US patient data is a HIPAA covered entity’s business associate. That means BAAs (Business Associate Agreements), and more importantly, it means your architecture has to be designed for HIPAA from day one, not retrofitted.
The things that catch teams late:
-
Encryption requirements:
PHI must be encrypted at rest and in transit. End-to-end encryption for data moving from device to cloud. AES-256 for stored data. TLS 1.2+ for all API integration communication. This sounds basic, but the edge cases are real — what happens to data buffered locally on a patient’s phone when they lose it? Does your app have remote wipe or device-level encryption enforcement?
-
Audit logging:
Every access to PHI needs to be logged. Who accessed which patient’s data, when, from which IP, what actions they took. This is not optional under HIPAA’s Security Rule. It also means your database schema needs audit tables or event sourcing from the start.
-
Access controls and minimum necessary:
Role-based access control (RBAC) isn’t enough for HIPAA — you need attribute-based access control (ABAC) for patient-provider relationships. A cardiologist should only see their assigned patients’ cardiac data, not all patients’ data.
-
Data retention and deletion:
HIPAA requires PHI retention for a minimum of 6 years. But patients also have rights to request deletion in some contexts. Your data lifecycle management needs to handle both, including backup systems.
-
Business Associate Agreements:
AWS, Azure, GCP, Twilio, Stripe — any vendor touching PHI needs a BAA. Major cloud vendors have BAA templates. Many SaaS tools don’t. Audit your entire vendor list.
If you’re building for the EU market or patients in multiple jurisdictions, add GDPR and potentially FDA SaMD (Software as a Medical Device) regulations to this list. The regulatory complexity multiplies fast.
The EngineerBabu team recommends a dedicated security and compliance sprint at the architecture phase — before development begins — not after your first pentest comes back with 47 findings.
EHR Integration: Where RPM Systems Stall
The most common late-stage problem I see in RPM development is EHR integration underestimation.
Health systems operate on Epic, Cerner, Allscripts, Athenahealth, and others. Getting RPM vitals data flowing into a patient’s EHR record is a clinical requirement for most enterprise clients. And EHR integration is genuinely hard.
The modern standard is HL7 FHIR R4 with SMART on FHIR for authentication. Epic and Cerner have FHIR-compliant APIs — but they’re sandboxed heavily, the production approval process takes 8-16 weeks for Epic specifically, and the data models for vitals (Observation resources, Device resources) have nuances that require clinical informatics knowledge.
Older integration methods (HL7 v2 over MLLP, direct database connections, middleware like Mirth Connect) still exist at many health systems and are messier to work with.
What I tell founders: scope EHR integration as a separate work stream with a 12-16 week runway, not a 2-week sprint at the end. Identify your target EHR vendor on day one. Get into their developer sandbox program immediately. The integration timeline is determined more by vendor approval processes than by your engineering capacity.
AI and Machine Learning in RPM: Where It’s Actually Useful
The question I get often: should we build AI into our RPM system?
My answer: yes, but for specific, narrow use cases where the model output is decision support, not clinical decision-making.
The AI features that actually add value in RPM today:
- Anomaly detection: ML models trained on a patient’s own historical baselines can detect deviations that static threshold rules miss. A heart rate of 105 bpm might be normal for one patient and alarming for another. Personalized baselines reduce alert fatigue significantly.
- Predictive deterioration models: Early warning scores (NEWS2, MEWS equivalents) adapted for home settings. Models that predict 24-72 hour deterioration risk from vitals trends. This is where the clinical value is high but the validation bar is also high.
- Alert fatigue reduction: ML-based alert prioritization that learns from which alerts clinicians act on and which they dismiss. This is an operational AI use case with lower regulatory burden than clinical prediction.
- Natural language documentation: LLM-assisted care notes that draft documentation from alert acknowledgments, reducing clinician documentation burden. This is becoming a differentiator.
What AI is NOT ready for in RPM: autonomous clinical decision-making, replacing human review, or anything marketed as diagnostic without going through FDA 510(k) or De Novo pathway.
If your RPM system includes AI features that influence clinical decisions, you’re almost certainly looking at FDA Software as a Medical Device (SaMD) classification. Build time for a regulatory pathway analysis before you write ML code.
Remote Patient Monitoring App Development Cost: Real Numbers
The question every founder asks. Here’s what I’ve seen across 15+ RPM builds at different complexity levels.
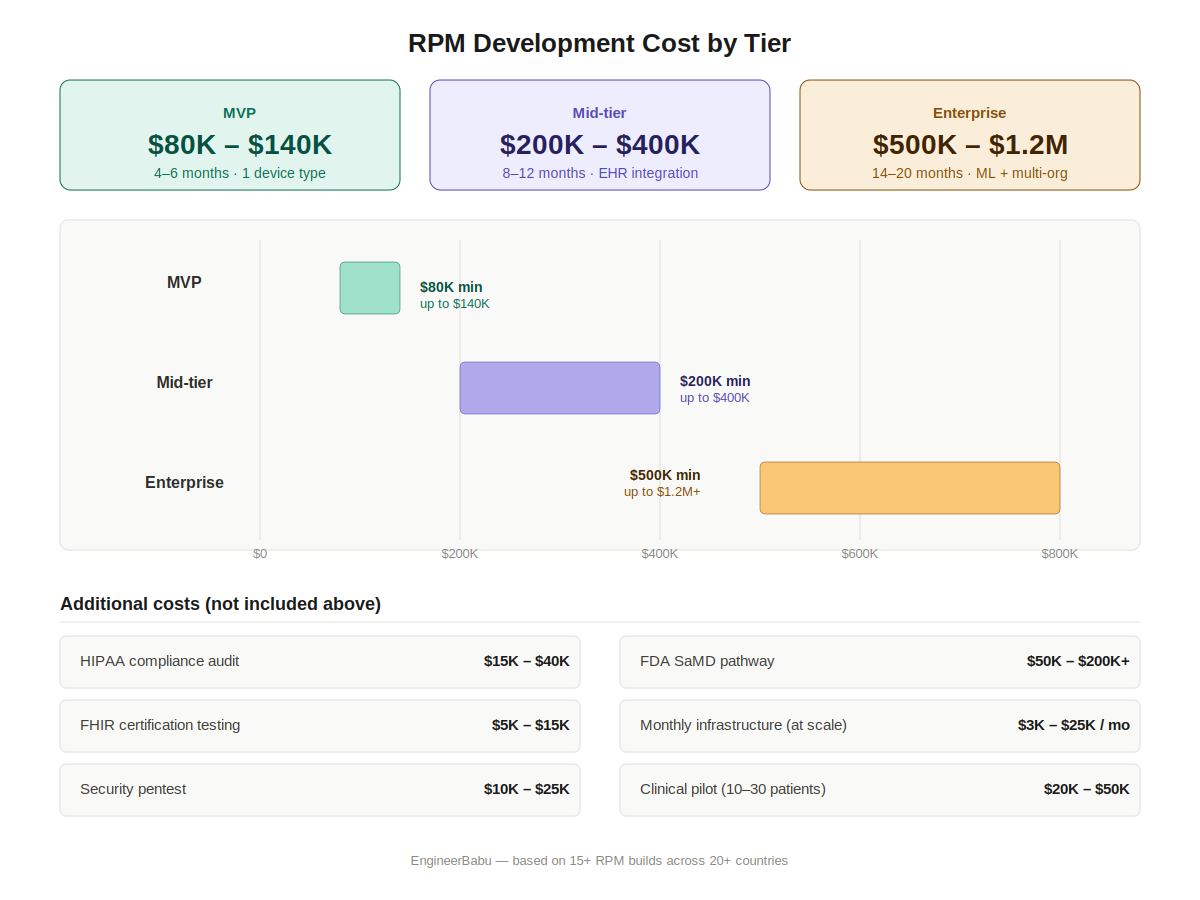
| System Complexity | Timeline | Cost Range (USD) |
| MVP (1 device type, basic vitals, alert SMS, simple dashboard) | 4-6 months | $80,000 – $140,000 |
| Mid-tier (3-5 device types, real-time streaming, EHR integration, care team dashboard) | 8-12 months | $200,000 – $400,000 |
| Enterprise (multi-org, custom clinical workflows, ML anomaly detection, full FHIR integration) | 14-20 months | $500,000 – $1,200,000 |
A few things those ranges don’t include:
- Regulatory/compliance consulting: Budget $15,000 – $40,000 for HIPAA compliance audit, BAA review, and security assessment
- FDA SaMD pathway (if applicable): $50,000 – $200,000+ depending on classification
- Device hardware certification (if you’re making your own hardware): This is a completely different cost category. FCC, FDA 510(k) for device, Bluetooth SIG qualification
- FHIR certification testing: $5,000 – $15,000
- Ongoing infrastructure: $3,000 – $25,000/month depending on patient volume and data retention
The numbers founders most consistently underestimate: compliance ($30K-$50K minimum), EHR integration (adds 2-3 months), and infrastructure costs after launch as patient volume scales.
What Most Founders Get Wrong About RPM Development
After seeing enough of these builds, patterns emerge. These are the mistakes I see repeatedly.
- Treating it as a standard mobile app project. RPM is an IoT + health informatics + compliance problem wearing a mobile app costume. Teams that scope it like a consumer app hit walls at device integration, data pipeline architecture, and compliance review. Typically this costs 3-4 months and $60,000-$100,000 in unplanned rework.
- Building alerts before building data quality. Alerts are only as good as the data triggering them. RPM data is inherently noisy — motion artifacts, connection drops, device calibration drift. Teams that build alert rules on raw data get overwhelmed with false positives, which destroys clinical trust in the system. Build a data quality and signal validation layer before you write a single alert rule.
- Underestimating HIPAA BAA lead time. You cannot onboard a healthcare enterprise client without a signed BAA in place. Getting BAAs from your vendors — and then presenting your own BAA to enterprise clients for their legal review — takes 4-8 weeks minimum. Teams that don’t start this process early end up delaying commercial launches by months.
- Designing the dashboard for patients instead of clinicians. The clinician-facing dashboard drives adoption and revenue. Patients don’t choose RPM platforms — care systems do. I’ve seen technically excellent RPM products fail commercially because the clinical workflow was designed by a product team that never spent a day in a clinical environment. Get your clinician users into design sessions from week one.
- Not designing for alert fatigue from day one. The leading reason healthcare systems abandon RPM programs is alert fatigue. If your system generates more noise than signal, clinicians stop trusting it. Design your alerting system with a clinical advisor who can help you establish meaningful, validated thresholds and suppression logic from the start.
Build vs. Buy: Evaluating RPM Platform Vendors
There are mature white-label RPM platforms available today — Current Health (now Best Buy Health), Biofourmis, Health Recovery Solutions, TytoCare, and others. For many health systems, the right answer is not custom development.
Here’s a simple framework I use with founders:
Build custom RPM when:
- You have a specific clinical protocol or device integration not supported by existing platforms
- You’re building a disease-specific solution (cardiac-specific, diabetes management, COPD) where depth beats breadth
- You need to own the data infrastructure for research, ML, or platform licensing downstream
- Your competitive differentiation IS the technology, not the clinical program around it
Buy/white-label when:
- Your differentiation is clinical program design and care management, not technology
- You need to be in market within 6 months
- Your patient volume doesn’t justify custom infrastructure costs
- You’re a health system, not a health-tech company
The hybrid path — building on top of an FDA-cleared RPM platform’s APIs while customizing the clinical workflow layer — is often underexplored. It’s worth mapping before committing to full custom development.
Remote Patient Monitoring App Development: Step-by-Step Process
For teams that have decided to build, here’s the process the EngineerBabu team follows:
- Clinical requirements workshop (weeks 1-2): Define clinical use case, patient population, vital parameters, alert protocols, care team workflows. This is done with clinical advisors, not just product teams.
- Regulatory and compliance scoping (weeks 2-3): Identify HIPAA, FDA SaMD, and international compliance requirements. Determine BAA requirements. Begin vendor BAA collection.
- Architecture design (weeks 3-5): Data freshness requirement, cloud infrastructure design, device integration strategy, FHIR/interoperability architecture, security architecture.
- Device integration sprint (weeks 5-9): Dedicated sprint for hardware SDK integration, BLE reliability testing, offline buffering, data quality layer. Run this parallel to nothing else.
- Core backend development (weeks 6-18): IoT ingestion, data pipeline, time-series storage, rules engine, FHIR API layer, notification service.
- Mobile app development (weeks 8-18): Patient app (iOS and Android development), background collection, secure local storage, sync engine.
- Care team dashboard (weeks 10-20): Web dashboard, multi-patient monitoring, alert management, audit trail.
- EHR integration (weeks 8-24): Start this work stream immediately. It runs in parallel but has the longest external dependency.
- Security audit and HIPAA assessment (weeks 20-22): Third-party pentest, HIPAA technical safeguard review, BAA finalization.
- Clinical pilot (weeks 22-28): 10-30 patient pilot with a clinical partner. Real data will surface issues your QA can’t.
The clinical pilot step is non-negotiable. Every RPM system I’ve seen that launched without a clinical pilot had expensive post-launch issues that a 6-week pilot would have caught.
The Architecture Review I Offer Before You Commit
If you’re evaluating remote patient monitoring app development and want to talk through the architecture decisions before you commit to a vendor or timeline, I’m usually the one on those calls.
The things I care about on those calls: your clinical use case, your data freshness requirement, your device strategy, your regulatory exposure, and whether your team structure matches what you’re trying to build.
No deck. No sales process. Just an honest conversation about whether what you’re planning will work.
You can reach me directly: mayank@engineerbabu.com
Mayank Pratap Co-founder, EngineerBabu, 14 years building technology products | Google AI Accelerator Top 20 (2024) | CMMI Level 5 | NASSCOM Member | 500+ projects delivered across 20+ countries.
FAQ: Remote Patient Monitoring App Development
-
What devices can a remote patient monitoring app integrate with?
Common integrations include pulse oximeters (Nonin, Masimo), blood pressure monitors (Omron, iHealth), glucometers (Dexcom, Abbott FreeStyle), weight scales (Withings), ECG patches (AliveCor KardiaMobile, BioTel Heart), thermometers, and spirometers.
Each device type has different SDK requirements, connectivity protocols (BLE, WiFi, cellular), and data formats. Most RPM platforms support 5-15 device types at launch; enterprise platforms may support 30+.
-
How long does it take to build a remote patient monitoring app?
A basic MVP with one device type, core vitals display, and SMS alerts takes 4-6 months. A production-ready system with real-time streaming, care team dashboard, and EHR integration typically takes 10-14 months. The single largest timeline variable is EHR integration — Epic production API approval alone takes 8-16 weeks.
-
Is HIPAA compliance required for all RPM apps?
If your RPM app transmits or stores individually identifiable health information and works with HIPAA-covered entities (hospitals, insurers, healthcare providers) or their business associates, HIPAA compliance is required.
This includes Business Associate Agreements with all vendors, technical safeguards for PHI, audit controls, and transmission security. Apps serving only individual consumers directly (not through a healthcare provider) operate under a different regulatory framework, though state-level health privacy laws still apply.