A pharmacy owner in Bangalore called me last year. They had just spent ₹28 lakhs on a custom pharmacy management system.
Six months in, the software couldn’t sync inventory across 3 branches, had no drug interaction alerts, and their GSTIN-compliant billing module was a separate tool that their team manually reconciled every evening.
The vendor had delivered “features.” They had not delivered a system.
I’ve reviewed the architecture of enough healthcare software projects at EngineerBabu to tell you exactly where pharmacy management system development falls apart. And it’s never the feature you’d expect.
EngineerBabu is a CMMI Level 5 certified product engineering company. We’ve built 500+ products across 20+ countries, 200+ of which were VC-funded.
When I’m evaluating a pharmacy software brief, I’m thinking about three things the vendor rarely mentions upfront.
Data architecture for regulatory audits, integration depth with the existing healthcare ecosystem, and the operational edge cases that surface only after 60 days of live usage.
This guide is the one I wish had existed when we took on our first pharma software project.
What Is Pharmacy Management System Development?
Pharmacy management system development is the process of designing, building, and deploying a digital platform that centralizes and automates pharmacy operations — from inventory tracking and prescription processing to billing, regulatory compliance, patient records, and multi-store coordination.
A modern PMS is not an inventory tool with a billing tab added to it. It is an interconnected system where the inventory engine, e-prescription module, EHR/EMR integration layer, insurance claims processor, and analytics dashboard talk to each other in real time.
That distinction determines 80% of whether your project succeeds or fails.
Why Pharmacy Software Development Is a Critical Investment Right Now
The global pharmacy management software market is valued at $101.07 billion in 2025 and is projected to reach $207.48 billion by 2030, growing at a CAGR of 15.47%, making it one of the fastest-scaling verticals in healthcare technology.
Cloud deployment now accounts for over 63% of market share and is expanding at a 17.5% CAGR.
Independent pharmacies still hold roughly 57% of the market, but chained pharmacies are growing at 17.1% annually.
What’s driving this?
It’s not just convenience. Regulatory pressure is intensifying. Prescription volumes are climbing. Margins are thin.
And patients now expect pharmacies to function as connected care hubs, not just pill counters.
AI-driven systems are enabling pharmacies to reduce inventory levels by around 20% through more accurate demand forecasting and optimized reorder strategies, according to a 2025 industry analysis from MindInventory.
That number alone justifies the development investment for any pharmacy running 500+ SKUs.
The Core Modules Your Pharmacy System Actually Needs
This is where most software briefs go wrong. Clients arrive with feature lists. Experienced engineering teams think in modules and data flows.
1. Inventory and Drug Supply Chain Management
This is the backbone of the entire system. Inventory management with real-time stock tracking, automated reorder triggers based on consumption patterns, expiry date monitoring, barcode scanner integration, and vendor management is a must.
For a chain pharmacy, add multi-warehouse visibility and stock transfer workflows.
The database design here matters enormously. If you store inventory as a flat table, you’ll hit scaling problems at around 2,000 SKUs.
You need a hierarchical structure that handles variants (generic vs. branded), lot numbers, and NDC codes cleanly.
2. Prescription Management and e-Prescribing
The e-prescribing market is expected to grow to $3.3 billion by 2025, growing at a CAGR of 23.3%. Your PMS needs to integrate with this ecosystem, not sit outside it.
A prescription module should handle digital prescription intake, pharmacist review queues, drug interaction alerts, dosage verification, and auto-refill scheduling.
The workflow matters as much as the features. One of the most common UX failures I’ve seen: systems that make pharmacists click through 7 screens to dispense a refill.
That’s not software, that’s an obstacle course.
3. Billing, Insurance Claims, and Revenue Cycle Management
This is where pharmacy owners feel the most pain from bad software. Insurance claim submission, eligibility verification, copay calculation, GST-compliant invoicing, A/R tracking, and denial management all need to work together.
For India-specific builds, you need Schedule H and Schedule H1 drug compliance baked into the billing module.
For US-facing platforms, HIPAA compliance and PBM (Pharmacy Benefits Management) integration are non-negotiable.
4. Patient Profile and CRM
Medication history, allergy alerts, refill reminders via SMS/WhatsApp, counseling notes, and patient engagement workflows.
The CRM layer is what separates a transactional pharmacy from one with meaningful patient retention.
5. Reporting, Analytics, and Business Intelligence
Purchase patterns, high-margin SKU identification, staff productivity metrics, expiry waste tracking, and regulatory audit trails.
The analytics layer is where pharmacy owners finally get visibility into a business they previously ran on gut feel.
6. Multi-Store Management (for chains)
Centralized inventory, branch-level P&L, inter-branch stock transfers, unified patient records, and role-based access control across locations.
This module alone adds 3-4 months to a build if not planned from the start.

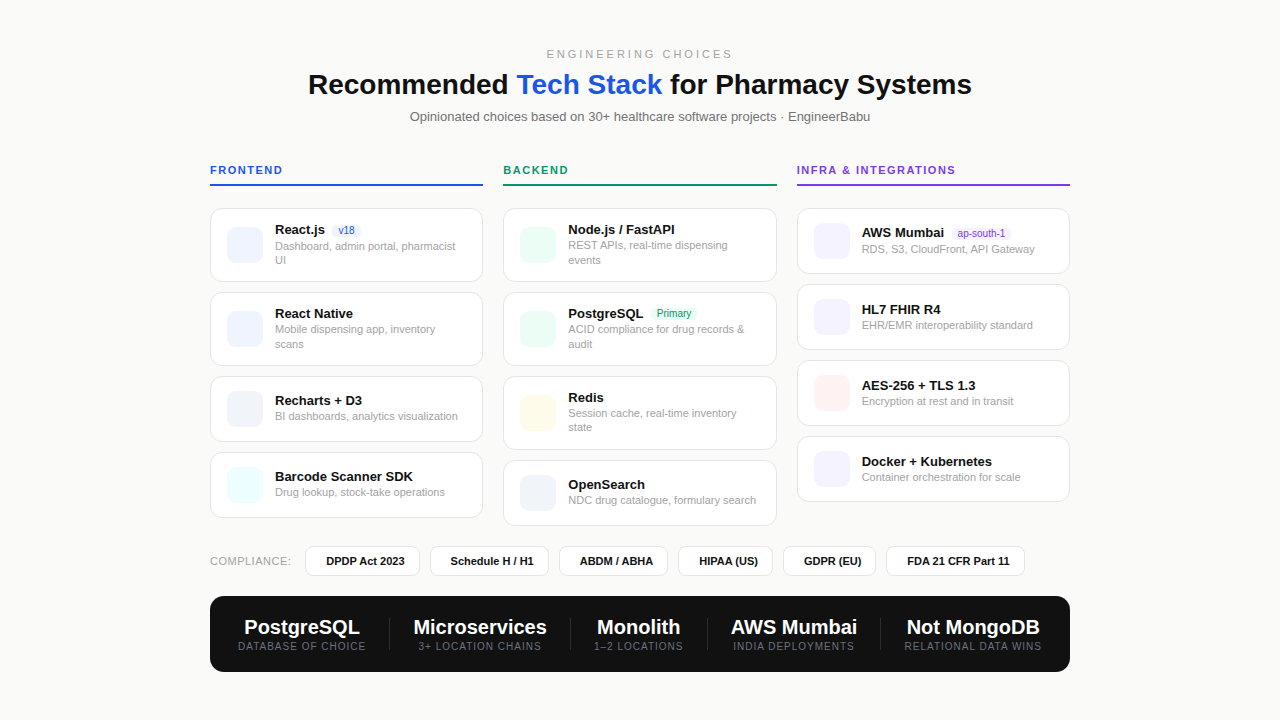
Technology Stack: What I’d Actually Choose
I’ll give you my honest opinion here, not a platform-neutral list.
-
Backend:
Node.js or Python (Django/FastAPI) for the application layer. PostgreSQL as the primary database — not MongoDB.
Pharmacy data has relational structure. Drug interactions, prescription linkages, inventory movements, patient histories — all of it benefits from ACID compliance and relational integrity.
I’ve seen teams pick MongoDB for pharmacy systems because it’s “flexible” and then spend 3 months retrofitting data consistency they could have had on day one.
-
Frontend:
React.js for the web dashboard. React Native if you need a mobile dispensing app.
Not a hybrid framework for the core pharmacy workflow — dispensing speed matters and native performance shows up here.
-
Architecture:
Microservices for chain pharmacies (3+ locations) and larger builds. A well-designed monolith with modular separation is perfectly fine for a single-location or two-location pharmacy.
Don’t build microservices complexity into a small pharmacy deployment. It adds infrastructure cost, operational overhead, and debugging complexity that the business doesn’t need.
-
Cloud:
AWS with RDS for managed PostgreSQL, S3 for document storage (prescriptions, audit trails), and CloudFront for the CDN layer.
If the client is India-focused and cost-sensitive, AWS Mumbai region gives good latency and reasonable pricing.
-
Integrations:
HL7 FHIR standards for EHR/EMR data exchange. ABDM (Ayushman Bharat Digital Mission) integration for India-specific builds.
REST APIs for insurance and PBM connections.
-
Security:
AES-256 encryption at rest, TLS 1.3 in transit, role-based access control at the database level (not just the application layer), full audit logging on every drug dispensation record, and penetration testing before go-live.
How Long Does Pharmacy Management System Development Take?
I’ll give you real numbers, not ranges wide enough to be useless.
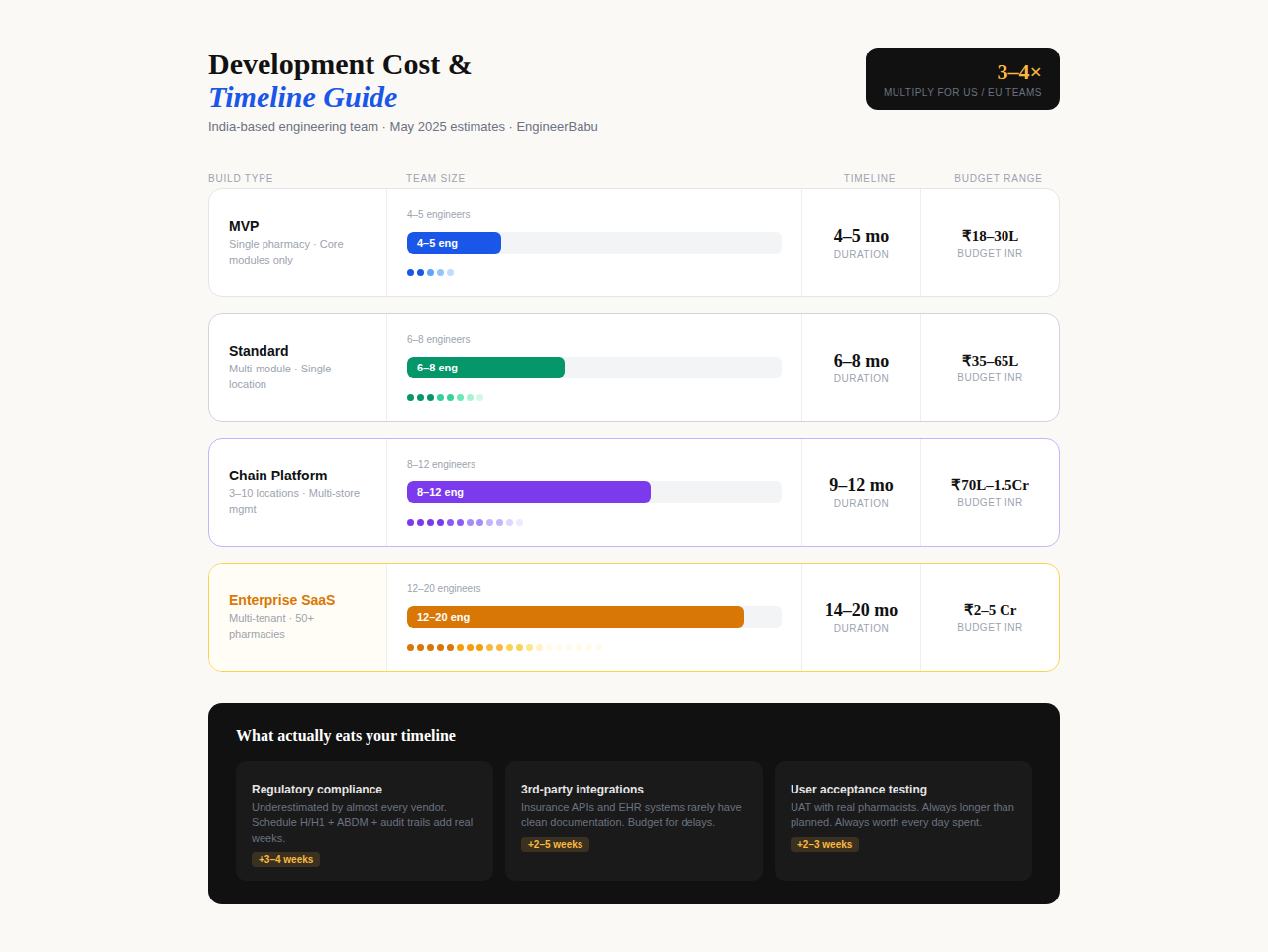
| Build Type | Timeline | Team Size | Budget Range (India) |
| MVP (single pharmacy, core modules) | 4-5 months | 4-5 engineers | ₹18-30 lakhs |
| Standard (multi-module, single location) | 6-8 months | 6-8 engineers | ₹35-65 lakhs |
| Chain pharmacy platform (3-10 locations) | 9-12 months | 8-12 engineers | ₹70-1.5 crore |
| Enterprise SaaS (multi-tenant, 50+ pharmacies) | 14-20 months | 12-20 engineers | ₹2-5 crore |
These numbers assume an India-based engineering team. For US or EU-based teams, multiply by roughly 3-4x.
The most common mistake I see in project scoping:
Clients budget for the MVP timeline but have enterprise feature expectations. That mismatch causes 70% of pharmacy software projects to run over budget.
What actually eats your timeline: regulatory compliance requirements (underestimated by 3-4 weeks in almost every project), third-party integration delays (insurance APIs and EHR systems rarely have clean documentation), and user acceptance testing with actual pharmacists (always longer than planned, always worth it).
Compliance and Regulatory Requirements You Cannot Skip
This section is where generic content blogs stop. I’ll go further.
1. India-specific compliance:
- Drugs and Cosmetics Act, 1940 — Schedule H, H1, and X drug records with mandatory 3-year retention
- DPDP Act (Digital Personal Data Protection Act, 2023) — affects how you store and process patient data
- ABDM integration for digital health ID linkage
- GST invoicing with HSN codes for pharmaceuticals
- State-specific drug license record requirements vary significantly by state.
2. Global compliance for SaaS platforms:
- HIPAA (US) — affects every layer: storage, transmission, access control, breach notification
- GDPR (EU) — data residency, consent management, right to erasure
- FDA 21 CFR Part 11 — electronic records and signatures for US pharmaceutical operations
- DSCSA (Drug Supply Chain Security Act) — serialization and traceability for the US drug supply chain
One thing I tell every healthcare client: build compliance into the architecture, not as an afterthought.
Adding HIPAA-grade audit logging to a system that wasn’t designed for it is a 2-3 month retrofit. Building it in from the start adds 3-4 weeks. The math is obvious.
What EngineerBabu Learned Building Healthcare Products at Scale
When the EngineerBabu team built OpenMoney’s neobank platform, one of the biggest challenges wasn’t the payment rails — it was the audit trail architecture.
Every financial transaction needed an immutable, timestamped record accessible to regulators on demand.
We built that at the database level, not the application level. The same principle applies to pharmacy systems, where every drug dispensation is a liability record.
For Simba Beer’s inventory intelligence platform, we built a real-time field data pipeline that gave their supply chain team visibility into stock movements across distribution points.
The learning there: real-time inventory isn’t a feature, it’s an infrastructure decision you make on day one.
Bolting real-time sync onto a batch-processing inventory system later is one of the most expensive refactors I’ve seen clients face.
Three things pharmacy software projects get wrong consistently:
-
First, they build inventory management, not inventory intelligence.
Tracking stock levels is table stakes. The value is in predicting stockouts 5-7 days before they happen, identifying slow-moving SKUs tying up working capital, and flagging expiry waste before it shows up in the P&L.
-
Second, they underestimate the pharmacist’s workflow
Every extra click in a high-volume dispensing environment costs real time and real money. A pharmacist dispensing 200 prescriptions a day who saves 15 seconds per transaction saves 50 minutes of labor daily.
I insist on pharmacist workflow observation sessions before any UI design starts.
-
Third, they skip the data migration plan
Most pharmacies switching to a new system have years of inventory data, patient records, and purchase histories in Excel, Tally, or a legacy system.
A clean migration strategy takes 3-4 weeks to plan and execute properly. Most vendors treat it as an afterthought and then own the consequences.
Build vs. Buy: The Decision Framework
This question deserves a direct answer.
Buy an off-the-shelf system when:
- You run 1-2 pharmacy locations with standard workflows
- You don’t need custom integrations with proprietary systems
- Your budget for development is under ₹15 lakhs
- You can live within the constraints of a vendor’s update cycle and feature roadmap
Good options: Marg ERP, Tally with pharma modules, WinPCS, or internationally, PioneerRx and Liberty Software.
Build custom when:
- You’re building a pharmacy chain (3+ locations) and need differentiated operational workflows
- You’re launching a pharmacy SaaS product for other pharmacies
- You need deep integration with hospital systems, insurance providers, or government health platforms
- Your pharmacy has a specialty focus (compounding, oncology, long-term care) with non-standard workflows
- You want to own your data and your roadmap without vendor dependency
The off-the-shelf vs. custom decision isn’t about features. It’s about whether your business model requires software that can evolve with you. If it does, custom is the only real answer.
What Most Teams Get Wrong About Pharmacy Software Development
After reviewing 30+ pharmacy and healthcare software projects, the pattern is clear.
The biggest mistake is treating pharmacy software as a standard CRUD application with a medical skin. It’s not.
The compliance layer is not a feature you add. The drug interaction engine is not a simple lookup table. The audit trail is not application-level logging. Every one of these decisions has liability implications.
The second mistake is building for the pharmacy owner’s vision of how the system should work, not how pharmacists actually work.
Pharmacy teams have developed workflows over years. Software that ignores those workflows gets abandoned or routed around.
The third is ignoring the integration surface area. A modern pharmacy system touches the
EHR of the hospital next door, the insurance portal of 12 different providers, the government’s drug licensing database, and potentially the patient’s health app.
Planning for those integrations on day one changes your architecture in fundamental ways. Discovering them in month 5 changes your budget in unfortunate ways.
The fourth, and the one I see most in India specifically: building for today’s pharmacy count. I’ve seen a pharmacy chain plan software for their current 4 locations, ship it, then hit 12 locations in 18 months and find their database schema can’t handle multi-tenancy.
Designing for scale you don’t yet have costs 15-20% more upfront and saves 3x that in retrofit costs.
Ready to Build?
If you’re evaluating pharmacy management system development and want to talk through the architecture decisions before you commit to a vendor or a spec, I’m usually the one on those calls at EngineerBabu.
Not a sales team. Not an account manager. Me.
We take 20 projects a year. Every client comes from a referral. If you’ve read this far, you’re already thinking about this the right way.
Write to me directly: mayank@engineerbabu.com
Or explore what the EngineerBabu team has built in healthcare and fintech at engineerbabu.com.
Mayank Pratap
Co-founder, EngineerBabu, 14 years building technology products | Google AI Accelerator Top 20 (2024) | CMMI Level 5 | NASSCOM Member | LinkedIn Top 20 Startups India
500+ projects delivered across 20+ countries | Backed by Vijay Shekhar Sharma (Paytm Founder)
FAQ
1. How much does it cost to develop a pharmacy management system in India?
The cost ranges from ₹18-30 lakhs for a single-pharmacy MVP with core modules to ₹70 lakhs to ₹1.5 crore for a chain pharmacy platform.
Enterprise SaaS products built for multiple pharmacy clients typically run ₹2-5 crore.
The biggest cost drivers are the number of third-party integrations, the compliance requirements (HIPAA, ABDM, etc.), and the level of real-time functionality needed.
2. How long does pharmacy management system development take?
A focused MVP takes 4-5 months with a team of 4-5 engineers. A full-featured multi-module system for a single pharmacy runs 6-8 months.
Chain pharmacy platforms with multi-store management and analytics take 9-12 months.
The timeline is heavily influenced by third-party integration complexity and regulatory compliance requirements, which most development vendors underestimate.
3. What technology stack is best for pharmacy management software?
For most pharmacy builds, React.js on the frontend, Node.js or Django on the backend, and PostgreSQL as the database is a strong, proven stack.
Microservices architecture makes sense for chain platforms serving 3+ locations; a modular monolith is more appropriate for smaller deployments.
Cloud hosting on AWS with Mumbai region works well for India-focused products.
4. Is HIPAA compliance necessary for Indian pharmacy software?
HIPAA applies to US-facing systems. For India, the relevant frameworks are the DPDP Act (2023), Schedule H/H1 drug record requirements under the Drugs and Cosmetics Act, and ABDM guidelines for digital health integration.
If you’re building a product that will serve international markets, HIPAA and GDPR compliance need to be planned from the architecture stage.
5. What are the must-have modules in a pharmacy management system?
The core modules are: inventory and drug supply chain management, prescription and e-prescribing workflow, billing and insurance claims processing, patient profile and CRM, and reporting and analytics.
For chain pharmacies, add a multi-store management module.
Most of these modules exist in every PMS brief — what differentiates a good system is how they integrate with each other and with external systems.